Have a language expert improve your writing
Run a free plagiarism check in 10 minutes, generate accurate citations for free.
- Knowledge Base
Methodology
- How to Write a Literature Review | Guide, Examples, & Templates

How to Write a Literature Review | Guide, Examples, & Templates
Published on January 2, 2023 by Shona McCombes . Revised on September 11, 2023.
What is a literature review? A literature review is a survey of scholarly sources on a specific topic. It provides an overview of current knowledge, allowing you to identify relevant theories, methods, and gaps in the existing research that you can later apply to your paper, thesis, or dissertation topic .
There are five key steps to writing a literature review:
- Search for relevant literature
- Evaluate sources
- Identify themes, debates, and gaps
- Outline the structure
- Write your literature review
A good literature review doesn’t just summarize sources—it analyzes, synthesizes , and critically evaluates to give a clear picture of the state of knowledge on the subject.
Instantly correct all language mistakes in your text
Upload your document to correct all your mistakes in minutes
Table of contents
What is the purpose of a literature review, examples of literature reviews, step 1 – search for relevant literature, step 2 – evaluate and select sources, step 3 – identify themes, debates, and gaps, step 4 – outline your literature review’s structure, step 5 – write your literature review, free lecture slides, other interesting articles, frequently asked questions, introduction.
- Quick Run-through
- Step 1 & 2
When you write a thesis , dissertation , or research paper , you will likely have to conduct a literature review to situate your research within existing knowledge. The literature review gives you a chance to:
- Demonstrate your familiarity with the topic and its scholarly context
- Develop a theoretical framework and methodology for your research
- Position your work in relation to other researchers and theorists
- Show how your research addresses a gap or contributes to a debate
- Evaluate the current state of research and demonstrate your knowledge of the scholarly debates around your topic.
Writing literature reviews is a particularly important skill if you want to apply for graduate school or pursue a career in research. We’ve written a step-by-step guide that you can follow below.
Prevent plagiarism. Run a free check.
Writing literature reviews can be quite challenging! A good starting point could be to look at some examples, depending on what kind of literature review you’d like to write.
- Example literature review #1: “Why Do People Migrate? A Review of the Theoretical Literature” ( Theoretical literature review about the development of economic migration theory from the 1950s to today.)
- Example literature review #2: “Literature review as a research methodology: An overview and guidelines” ( Methodological literature review about interdisciplinary knowledge acquisition and production.)
- Example literature review #3: “The Use of Technology in English Language Learning: A Literature Review” ( Thematic literature review about the effects of technology on language acquisition.)
- Example literature review #4: “Learners’ Listening Comprehension Difficulties in English Language Learning: A Literature Review” ( Chronological literature review about how the concept of listening skills has changed over time.)
You can also check out our templates with literature review examples and sample outlines at the links below.
Download Word doc Download Google doc
Before you begin searching for literature, you need a clearly defined topic .
If you are writing the literature review section of a dissertation or research paper, you will search for literature related to your research problem and questions .
Make a list of keywords
Start by creating a list of keywords related to your research question. Include each of the key concepts or variables you’re interested in, and list any synonyms and related terms. You can add to this list as you discover new keywords in the process of your literature search.
- Social media, Facebook, Instagram, Twitter, Snapchat, TikTok
- Body image, self-perception, self-esteem, mental health
- Generation Z, teenagers, adolescents, youth
Search for relevant sources
Use your keywords to begin searching for sources. Some useful databases to search for journals and articles include:
- Your university’s library catalogue
- Google Scholar
- Project Muse (humanities and social sciences)
- Medline (life sciences and biomedicine)
- EconLit (economics)
- Inspec (physics, engineering and computer science)
You can also use boolean operators to help narrow down your search.
Make sure to read the abstract to find out whether an article is relevant to your question. When you find a useful book or article, you can check the bibliography to find other relevant sources.
You likely won’t be able to read absolutely everything that has been written on your topic, so it will be necessary to evaluate which sources are most relevant to your research question.
For each publication, ask yourself:
- What question or problem is the author addressing?
- What are the key concepts and how are they defined?
- What are the key theories, models, and methods?
- Does the research use established frameworks or take an innovative approach?
- What are the results and conclusions of the study?
- How does the publication relate to other literature in the field? Does it confirm, add to, or challenge established knowledge?
- What are the strengths and weaknesses of the research?
Make sure the sources you use are credible , and make sure you read any landmark studies and major theories in your field of research.
You can use our template to summarize and evaluate sources you’re thinking about using. Click on either button below to download.
Take notes and cite your sources
As you read, you should also begin the writing process. Take notes that you can later incorporate into the text of your literature review.
It is important to keep track of your sources with citations to avoid plagiarism . It can be helpful to make an annotated bibliography , where you compile full citation information and write a paragraph of summary and analysis for each source. This helps you remember what you read and saves time later in the process.
Receive feedback on language, structure, and formatting
Professional editors proofread and edit your paper by focusing on:
- Academic style
- Vague sentences
- Style consistency
See an example

To begin organizing your literature review’s argument and structure, be sure you understand the connections and relationships between the sources you’ve read. Based on your reading and notes, you can look for:
- Trends and patterns (in theory, method or results): do certain approaches become more or less popular over time?
- Themes: what questions or concepts recur across the literature?
- Debates, conflicts and contradictions: where do sources disagree?
- Pivotal publications: are there any influential theories or studies that changed the direction of the field?
- Gaps: what is missing from the literature? Are there weaknesses that need to be addressed?
This step will help you work out the structure of your literature review and (if applicable) show how your own research will contribute to existing knowledge.
- Most research has focused on young women.
- There is an increasing interest in the visual aspects of social media.
- But there is still a lack of robust research on highly visual platforms like Instagram and Snapchat—this is a gap that you could address in your own research.
There are various approaches to organizing the body of a literature review. Depending on the length of your literature review, you can combine several of these strategies (for example, your overall structure might be thematic, but each theme is discussed chronologically).
Chronological
The simplest approach is to trace the development of the topic over time. However, if you choose this strategy, be careful to avoid simply listing and summarizing sources in order.
Try to analyze patterns, turning points and key debates that have shaped the direction of the field. Give your interpretation of how and why certain developments occurred.
If you have found some recurring central themes, you can organize your literature review into subsections that address different aspects of the topic.
For example, if you are reviewing literature about inequalities in migrant health outcomes, key themes might include healthcare policy, language barriers, cultural attitudes, legal status, and economic access.
Methodological
If you draw your sources from different disciplines or fields that use a variety of research methods , you might want to compare the results and conclusions that emerge from different approaches. For example:
- Look at what results have emerged in qualitative versus quantitative research
- Discuss how the topic has been approached by empirical versus theoretical scholarship
- Divide the literature into sociological, historical, and cultural sources
Theoretical
A literature review is often the foundation for a theoretical framework . You can use it to discuss various theories, models, and definitions of key concepts.
You might argue for the relevance of a specific theoretical approach, or combine various theoretical concepts to create a framework for your research.
Like any other academic text , your literature review should have an introduction , a main body, and a conclusion . What you include in each depends on the objective of your literature review.
The introduction should clearly establish the focus and purpose of the literature review.
Depending on the length of your literature review, you might want to divide the body into subsections. You can use a subheading for each theme, time period, or methodological approach.
As you write, you can follow these tips:
- Summarize and synthesize: give an overview of the main points of each source and combine them into a coherent whole
- Analyze and interpret: don’t just paraphrase other researchers — add your own interpretations where possible, discussing the significance of findings in relation to the literature as a whole
- Critically evaluate: mention the strengths and weaknesses of your sources
- Write in well-structured paragraphs: use transition words and topic sentences to draw connections, comparisons and contrasts
In the conclusion, you should summarize the key findings you have taken from the literature and emphasize their significance.
When you’ve finished writing and revising your literature review, don’t forget to proofread thoroughly before submitting. Not a language expert? Check out Scribbr’s professional proofreading services !
This article has been adapted into lecture slides that you can use to teach your students about writing a literature review.
Scribbr slides are free to use, customize, and distribute for educational purposes.
Open Google Slides Download PowerPoint
If you want to know more about the research process , methodology , research bias , or statistics , make sure to check out some of our other articles with explanations and examples.
- Sampling methods
- Simple random sampling
- Stratified sampling
- Cluster sampling
- Likert scales
- Reproducibility
Statistics
- Null hypothesis
- Statistical power
- Probability distribution
- Effect size
- Poisson distribution
Research bias
- Optimism bias
- Cognitive bias
- Implicit bias
- Hawthorne effect
- Anchoring bias
- Explicit bias
A literature review is a survey of scholarly sources (such as books, journal articles, and theses) related to a specific topic or research question .
It is often written as part of a thesis, dissertation , or research paper , in order to situate your work in relation to existing knowledge.
There are several reasons to conduct a literature review at the beginning of a research project:
- To familiarize yourself with the current state of knowledge on your topic
- To ensure that you’re not just repeating what others have already done
- To identify gaps in knowledge and unresolved problems that your research can address
- To develop your theoretical framework and methodology
- To provide an overview of the key findings and debates on the topic
Writing the literature review shows your reader how your work relates to existing research and what new insights it will contribute.
The literature review usually comes near the beginning of your thesis or dissertation . After the introduction , it grounds your research in a scholarly field and leads directly to your theoretical framework or methodology .
A literature review is a survey of credible sources on a topic, often used in dissertations , theses, and research papers . Literature reviews give an overview of knowledge on a subject, helping you identify relevant theories and methods, as well as gaps in existing research. Literature reviews are set up similarly to other academic texts , with an introduction , a main body, and a conclusion .
An annotated bibliography is a list of source references that has a short description (called an annotation ) for each of the sources. It is often assigned as part of the research process for a paper .
Cite this Scribbr article
If you want to cite this source, you can copy and paste the citation or click the “Cite this Scribbr article” button to automatically add the citation to our free Citation Generator.
McCombes, S. (2023, September 11). How to Write a Literature Review | Guide, Examples, & Templates. Scribbr. Retrieved August 5, 2024, from https://www.scribbr.com/dissertation/literature-review/
Is this article helpful?
Shona McCombes
Other students also liked, what is a theoretical framework | guide to organizing, what is a research methodology | steps & tips, how to write a research proposal | examples & templates, get unlimited documents corrected.
✔ Free APA citation check included ✔ Unlimited document corrections ✔ Specialized in correcting academic texts
Purdue Online Writing Lab Purdue OWL® College of Liberal Arts
Writing a Literature Review

Welcome to the Purdue OWL
This page is brought to you by the OWL at Purdue University. When printing this page, you must include the entire legal notice.
Copyright ©1995-2018 by The Writing Lab & The OWL at Purdue and Purdue University. All rights reserved. This material may not be published, reproduced, broadcast, rewritten, or redistributed without permission. Use of this site constitutes acceptance of our terms and conditions of fair use.
A literature review is a document or section of a document that collects key sources on a topic and discusses those sources in conversation with each other (also called synthesis ). The lit review is an important genre in many disciplines, not just literature (i.e., the study of works of literature such as novels and plays). When we say “literature review” or refer to “the literature,” we are talking about the research ( scholarship ) in a given field. You will often see the terms “the research,” “the scholarship,” and “the literature” used mostly interchangeably.
Where, when, and why would I write a lit review?
There are a number of different situations where you might write a literature review, each with slightly different expectations; different disciplines, too, have field-specific expectations for what a literature review is and does. For instance, in the humanities, authors might include more overt argumentation and interpretation of source material in their literature reviews, whereas in the sciences, authors are more likely to report study designs and results in their literature reviews; these differences reflect these disciplines’ purposes and conventions in scholarship. You should always look at examples from your own discipline and talk to professors or mentors in your field to be sure you understand your discipline’s conventions, for literature reviews as well as for any other genre.
A literature review can be a part of a research paper or scholarly article, usually falling after the introduction and before the research methods sections. In these cases, the lit review just needs to cover scholarship that is important to the issue you are writing about; sometimes it will also cover key sources that informed your research methodology.
Lit reviews can also be standalone pieces, either as assignments in a class or as publications. In a class, a lit review may be assigned to help students familiarize themselves with a topic and with scholarship in their field, get an idea of the other researchers working on the topic they’re interested in, find gaps in existing research in order to propose new projects, and/or develop a theoretical framework and methodology for later research. As a publication, a lit review usually is meant to help make other scholars’ lives easier by collecting and summarizing, synthesizing, and analyzing existing research on a topic. This can be especially helpful for students or scholars getting into a new research area, or for directing an entire community of scholars toward questions that have not yet been answered.
What are the parts of a lit review?
Most lit reviews use a basic introduction-body-conclusion structure; if your lit review is part of a larger paper, the introduction and conclusion pieces may be just a few sentences while you focus most of your attention on the body. If your lit review is a standalone piece, the introduction and conclusion take up more space and give you a place to discuss your goals, research methods, and conclusions separately from where you discuss the literature itself.
Introduction:
- An introductory paragraph that explains what your working topic and thesis is
- A forecast of key topics or texts that will appear in the review
- Potentially, a description of how you found sources and how you analyzed them for inclusion and discussion in the review (more often found in published, standalone literature reviews than in lit review sections in an article or research paper)
- Summarize and synthesize: Give an overview of the main points of each source and combine them into a coherent whole
- Analyze and interpret: Don’t just paraphrase other researchers – add your own interpretations where possible, discussing the significance of findings in relation to the literature as a whole
- Critically Evaluate: Mention the strengths and weaknesses of your sources
- Write in well-structured paragraphs: Use transition words and topic sentence to draw connections, comparisons, and contrasts.
Conclusion:
- Summarize the key findings you have taken from the literature and emphasize their significance
- Connect it back to your primary research question
How should I organize my lit review?
Lit reviews can take many different organizational patterns depending on what you are trying to accomplish with the review. Here are some examples:
- Chronological : The simplest approach is to trace the development of the topic over time, which helps familiarize the audience with the topic (for instance if you are introducing something that is not commonly known in your field). If you choose this strategy, be careful to avoid simply listing and summarizing sources in order. Try to analyze the patterns, turning points, and key debates that have shaped the direction of the field. Give your interpretation of how and why certain developments occurred (as mentioned previously, this may not be appropriate in your discipline — check with a teacher or mentor if you’re unsure).
- Thematic : If you have found some recurring central themes that you will continue working with throughout your piece, you can organize your literature review into subsections that address different aspects of the topic. For example, if you are reviewing literature about women and religion, key themes can include the role of women in churches and the religious attitude towards women.
- Qualitative versus quantitative research
- Empirical versus theoretical scholarship
- Divide the research by sociological, historical, or cultural sources
- Theoretical : In many humanities articles, the literature review is the foundation for the theoretical framework. You can use it to discuss various theories, models, and definitions of key concepts. You can argue for the relevance of a specific theoretical approach or combine various theorical concepts to create a framework for your research.
What are some strategies or tips I can use while writing my lit review?
Any lit review is only as good as the research it discusses; make sure your sources are well-chosen and your research is thorough. Don’t be afraid to do more research if you discover a new thread as you’re writing. More info on the research process is available in our "Conducting Research" resources .
As you’re doing your research, create an annotated bibliography ( see our page on the this type of document ). Much of the information used in an annotated bibliography can be used also in a literature review, so you’ll be not only partially drafting your lit review as you research, but also developing your sense of the larger conversation going on among scholars, professionals, and any other stakeholders in your topic.
Usually you will need to synthesize research rather than just summarizing it. This means drawing connections between sources to create a picture of the scholarly conversation on a topic over time. Many student writers struggle to synthesize because they feel they don’t have anything to add to the scholars they are citing; here are some strategies to help you:
- It often helps to remember that the point of these kinds of syntheses is to show your readers how you understand your research, to help them read the rest of your paper.
- Writing teachers often say synthesis is like hosting a dinner party: imagine all your sources are together in a room, discussing your topic. What are they saying to each other?
- Look at the in-text citations in each paragraph. Are you citing just one source for each paragraph? This usually indicates summary only. When you have multiple sources cited in a paragraph, you are more likely to be synthesizing them (not always, but often
- Read more about synthesis here.
The most interesting literature reviews are often written as arguments (again, as mentioned at the beginning of the page, this is discipline-specific and doesn’t work for all situations). Often, the literature review is where you can establish your research as filling a particular gap or as relevant in a particular way. You have some chance to do this in your introduction in an article, but the literature review section gives a more extended opportunity to establish the conversation in the way you would like your readers to see it. You can choose the intellectual lineage you would like to be part of and whose definitions matter most to your thinking (mostly humanities-specific, but this goes for sciences as well). In addressing these points, you argue for your place in the conversation, which tends to make the lit review more compelling than a simple reporting of other sources.
- Resources Home 🏠
- Try SciSpace Copilot
- Search research papers
- Add Copilot Extension
- Try AI Detector
- Try Paraphraser
- Try Citation Generator
- April Papers
- June Papers
- July Papers

How To Write A Literature Review - A Complete Guide

Table of Contents
A literature review is much more than just another section in your research paper. It forms the very foundation of your research. It is a formal piece of writing where you analyze the existing theoretical framework, principles, and assumptions and use that as a base to shape your approach to the research question.
Curating and drafting a solid literature review section not only lends more credibility to your research paper but also makes your research tighter and better focused. But, writing literature reviews is a difficult task. It requires extensive reading, plus you have to consider market trends and technological and political changes, which tend to change in the blink of an eye.
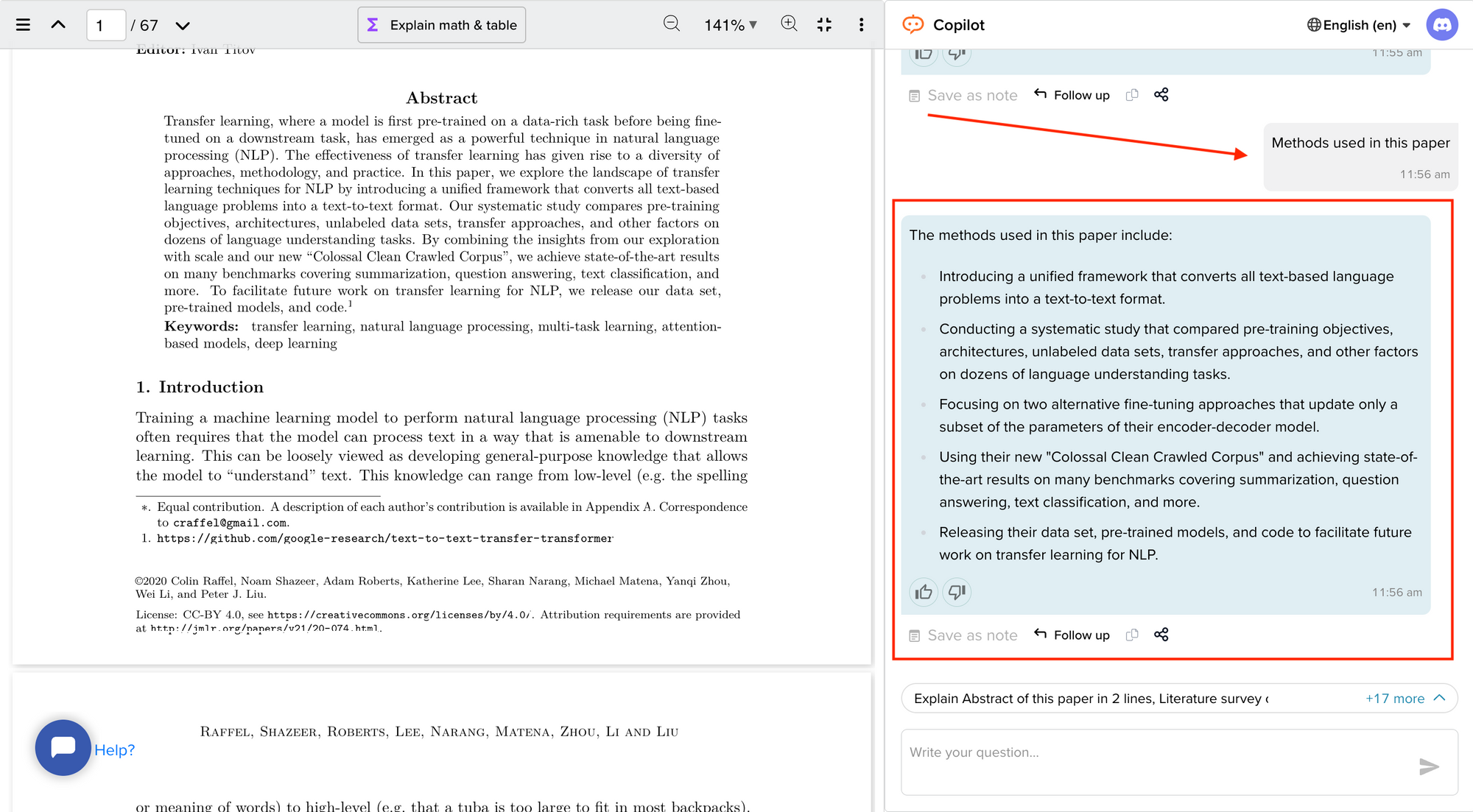
Now streamline your literature review process with the help of SciSpace Copilot. With this AI research assistant, you can efficiently synthesize and analyze a vast amount of information, identify key themes and trends, and uncover gaps in the existing research. Get real-time explanations, summaries, and answers to your questions for the paper you're reviewing, making navigating and understanding the complex literature landscape easier.
In this comprehensive guide, we will explore everything from the definition of a literature review, its appropriate length, various types of literature reviews, and how to write one.
What is a literature review?
A literature review is a collation of survey, research, critical evaluation, and assessment of the existing literature in a preferred domain.
Eminent researcher and academic Arlene Fink, in her book Conducting Research Literature Reviews , defines it as the following:
“A literature review surveys books, scholarly articles, and any other sources relevant to a particular issue, area of research, or theory, and by so doing, provides a description, summary, and critical evaluation of these works in relation to the research problem being investigated.
Literature reviews are designed to provide an overview of sources you have explored while researching a particular topic, and to demonstrate to your readers how your research fits within a larger field of study.”
Simply put, a literature review can be defined as a critical discussion of relevant pre-existing research around your research question and carving out a definitive place for your study in the existing body of knowledge. Literature reviews can be presented in multiple ways: a section of an article, the whole research paper itself, or a chapter of your thesis.
A literature review does function as a summary of sources, but it also allows you to analyze further, interpret, and examine the stated theories, methods, viewpoints, and, of course, the gaps in the existing content.
As an author, you can discuss and interpret the research question and its various aspects and debate your adopted methods to support the claim.
What is the purpose of a literature review?
A literature review is meant to help your readers understand the relevance of your research question and where it fits within the existing body of knowledge. As a researcher, you should use it to set the context, build your argument, and establish the need for your study.
What is the importance of a literature review?
The literature review is a critical part of research papers because it helps you:
- Gain an in-depth understanding of your research question and the surrounding area
- Convey that you have a thorough understanding of your research area and are up-to-date with the latest changes and advancements
- Establish how your research is connected or builds on the existing body of knowledge and how it could contribute to further research
- Elaborate on the validity and suitability of your theoretical framework and research methodology
- Identify and highlight gaps and shortcomings in the existing body of knowledge and how things need to change
- Convey to readers how your study is different or how it contributes to the research area
How long should a literature review be?
Ideally, the literature review should take up 15%-40% of the total length of your manuscript. So, if you have a 10,000-word research paper, the minimum word count could be 1500.
Your literature review format depends heavily on the kind of manuscript you are writing — an entire chapter in case of doctoral theses, a part of the introductory section in a research article, to a full-fledged review article that examines the previously published research on a topic.
Another determining factor is the type of research you are doing. The literature review section tends to be longer for secondary research projects than primary research projects.
What are the different types of literature reviews?
All literature reviews are not the same. There are a variety of possible approaches that you can take. It all depends on the type of research you are pursuing.
Here are the different types of literature reviews:
Argumentative review
It is called an argumentative review when you carefully present literature that only supports or counters a specific argument or premise to establish a viewpoint.
Integrative review
It is a type of literature review focused on building a comprehensive understanding of a topic by combining available theoretical frameworks and empirical evidence.
Methodological review
This approach delves into the ''how'' and the ''what" of the research question — you cannot look at the outcome in isolation; you should also review the methodology used.
Systematic review
This form consists of an overview of existing evidence pertinent to a clearly formulated research question, which uses pre-specified and standardized methods to identify and critically appraise relevant research and collect, report, and analyze data from the studies included in the review.
Meta-analysis review
Meta-analysis uses statistical methods to summarize the results of independent studies. By combining information from all relevant studies, meta-analysis can provide more precise estimates of the effects than those derived from the individual studies included within a review.
Historical review
Historical literature reviews focus on examining research throughout a period, often starting with the first time an issue, concept, theory, or phenomenon emerged in the literature, then tracing its evolution within the scholarship of a discipline. The purpose is to place research in a historical context to show familiarity with state-of-the-art developments and identify future research's likely directions.
Theoretical Review
This form aims to examine the corpus of theory accumulated regarding an issue, concept, theory, and phenomenon. The theoretical literature review helps to establish what theories exist, the relationships between them, the degree the existing approaches have been investigated, and to develop new hypotheses to be tested.
Scoping Review
The Scoping Review is often used at the beginning of an article, dissertation, or research proposal. It is conducted before the research to highlight gaps in the existing body of knowledge and explains why the project should be greenlit.
State-of-the-Art Review
The State-of-the-Art review is conducted periodically, focusing on the most recent research. It describes what is currently known, understood, or agreed upon regarding the research topic and highlights where there are still disagreements.
Can you use the first person in a literature review?
When writing literature reviews, you should avoid the usage of first-person pronouns. It means that instead of "I argue that" or "we argue that," the appropriate expression would be "this research paper argues that."
Do you need an abstract for a literature review?
Ideally, yes. It is always good to have a condensed summary that is self-contained and independent of the rest of your review. As for how to draft one, you can follow the same fundamental idea when preparing an abstract for a literature review. It should also include:
- The research topic and your motivation behind selecting it
- A one-sentence thesis statement
- An explanation of the kinds of literature featured in the review
- Summary of what you've learned
- Conclusions you drew from the literature you reviewed
- Potential implications and future scope for research
Here's an example of the abstract of a literature review
Is a literature review written in the past tense?
Yes, the literature review should ideally be written in the past tense. You should not use the present or future tense when writing one. The exceptions are when you have statements describing events that happened earlier than the literature you are reviewing or events that are currently occurring; then, you can use the past perfect or present perfect tenses.
How many sources for a literature review?
There are multiple approaches to deciding how many sources to include in a literature review section. The first approach would be to look level you are at as a researcher. For instance, a doctoral thesis might need 60+ sources. In contrast, you might only need to refer to 5-15 sources at the undergraduate level.
The second approach is based on the kind of literature review you are doing — whether it is merely a chapter of your paper or if it is a self-contained paper in itself. When it is just a chapter, sources should equal the total number of pages in your article's body. In the second scenario, you need at least three times as many sources as there are pages in your work.
Quick tips on how to write a literature review
To know how to write a literature review, you must clearly understand its impact and role in establishing your work as substantive research material.
You need to follow the below-mentioned steps, to write a literature review:
- Outline the purpose behind the literature review
- Search relevant literature
- Examine and assess the relevant resources
- Discover connections by drawing deep insights from the resources
- Structure planning to write a good literature review
1. Outline and identify the purpose of a literature review
As a first step on how to write a literature review, you must know what the research question or topic is and what shape you want your literature review to take. Ensure you understand the research topic inside out, or else seek clarifications. You must be able to the answer below questions before you start:
- How many sources do I need to include?
- What kind of sources should I analyze?
- How much should I critically evaluate each source?
- Should I summarize, synthesize or offer a critique of the sources?
- Do I need to include any background information or definitions?
Additionally, you should know that the narrower your research topic is, the swifter it will be for you to restrict the number of sources to be analyzed.
2. Search relevant literature
Dig deeper into search engines to discover what has already been published around your chosen topic. Make sure you thoroughly go through appropriate reference sources like books, reports, journal articles, government docs, and web-based resources.
You must prepare a list of keywords and their different variations. You can start your search from any library’s catalog, provided you are an active member of that institution. The exact keywords can be extended to widen your research over other databases and academic search engines like:
- Google Scholar
- Microsoft Academic
- Science.gov
Besides, it is not advisable to go through every resource word by word. Alternatively, what you can do is you can start by reading the abstract and then decide whether that source is relevant to your research or not.
Additionally, you must spend surplus time assessing the quality and relevance of resources. It would help if you tried preparing a list of citations to ensure that there lies no repetition of authors, publications, or articles in the literature review.
3. Examine and assess the sources
It is nearly impossible for you to go through every detail in the research article. So rather than trying to fetch every detail, you have to analyze and decide which research sources resemble closest and appear relevant to your chosen domain.
While analyzing the sources, you should look to find out answers to questions like:
- What question or problem has the author been describing and debating?
- What is the definition of critical aspects?
- How well the theories, approach, and methodology have been explained?
- Whether the research theory used some conventional or new innovative approach?
- How relevant are the key findings of the work?
- In what ways does it relate to other sources on the same topic?
- What challenges does this research paper pose to the existing theory
- What are the possible contributions or benefits it adds to the subject domain?
Be always mindful that you refer only to credible and authentic resources. It would be best if you always take references from different publications to validate your theory.
Always keep track of important information or data you can present in your literature review right from the beginning. It will help steer your path from any threats of plagiarism and also make it easier to curate an annotated bibliography or reference section.
4. Discover connections
At this stage, you must start deciding on the argument and structure of your literature review. To accomplish this, you must discover and identify the relations and connections between various resources while drafting your abstract.
A few aspects that you should be aware of while writing a literature review include:
- Rise to prominence: Theories and methods that have gained reputation and supporters over time.
- Constant scrutiny: Concepts or theories that repeatedly went under examination.
- Contradictions and conflicts: Theories, both the supporting and the contradictory ones, for the research topic.
- Knowledge gaps: What exactly does it fail to address, and how to bridge them with further research?
- Influential resources: Significant research projects available that have been upheld as milestones or perhaps, something that can modify the current trends
Once you join the dots between various past research works, it will be easier for you to draw a conclusion and identify your contribution to the existing knowledge base.
5. Structure planning to write a good literature review
There exist different ways towards planning and executing the structure of a literature review. The format of a literature review varies and depends upon the length of the research.
Like any other research paper, the literature review format must contain three sections: introduction, body, and conclusion. The goals and objectives of the research question determine what goes inside these three sections.
Nevertheless, a good literature review can be structured according to the chronological, thematic, methodological, or theoretical framework approach.
Literature review samples
1. Standalone
2. As a section of a research paper
How SciSpace Discover makes literature review a breeze?
SciSpace Discover is a one-stop solution to do an effective literature search and get barrier-free access to scientific knowledge. It is an excellent repository where you can find millions of only peer-reviewed articles and full-text PDF files. Here’s more on how you can use it:
Find the right information
Find what you want quickly and easily with comprehensive search filters that let you narrow down papers according to PDF availability, year of publishing, document type, and affiliated institution. Moreover, you can sort the results based on the publishing date, citation count, and relevance.
Assess credibility of papers quickly
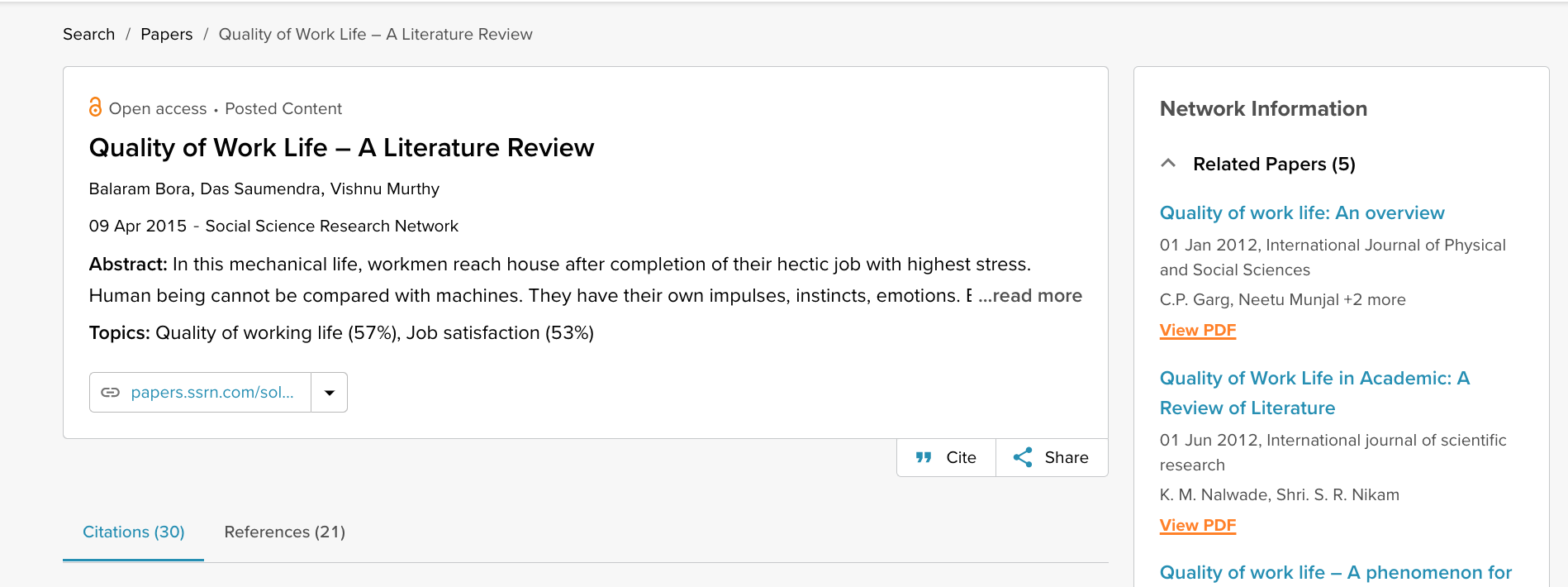
When doing the literature review, it is critical to establish the quality of your sources. They form the foundation of your research. SciSpace Discover helps you assess the quality of a source by providing an overview of its references, citations, and performance metrics.
Get the complete picture in no time
SciSpace Discover’s personalized suggestion engine helps you stay on course and get the complete picture of the topic from one place. Every time you visit an article page, it provides you links to related papers. Besides that, it helps you understand what’s trending, who are the top authors, and who are the leading publishers on a topic.
Make referring sources super easy
To ensure you don't lose track of your sources, you must start noting down your references when doing the literature review. SciSpace Discover makes this step effortless. Click the 'cite' button on an article page, and you will receive preloaded citation text in multiple styles — all you've to do is copy-paste it into your manuscript.
Final tips on how to write a literature review
A massive chunk of time and effort is required to write a good literature review. But, if you go about it systematically, you'll be able to save a ton of time and build a solid foundation for your research.
We hope this guide has helped you answer several key questions you have about writing literature reviews.
Would you like to explore SciSpace Discover and kick off your literature search right away? You can get started here .
Frequently Asked Questions (FAQs)
1. how to start a literature review.
• What questions do you want to answer?
• What sources do you need to answer these questions?
• What information do these sources contain?
• How can you use this information to answer your questions?
2. What to include in a literature review?
• A brief background of the problem or issue
• What has previously been done to address the problem or issue
• A description of what you will do in your project
• How this study will contribute to research on the subject
3. Why literature review is important?
The literature review is an important part of any research project because it allows the writer to look at previous studies on a topic and determine existing gaps in the literature, as well as what has already been done. It will also help them to choose the most appropriate method for their own study.
4. How to cite a literature review in APA format?
To cite a literature review in APA style, you need to provide the author's name, the title of the article, and the year of publication. For example: Patel, A. B., & Stokes, G. S. (2012). The relationship between personality and intelligence: A meta-analysis of longitudinal research. Personality and Individual Differences, 53(1), 16-21
5. What are the components of a literature review?
• A brief introduction to the topic, including its background and context. The introduction should also include a rationale for why the study is being conducted and what it will accomplish.
• A description of the methodologies used in the study. This can include information about data collection methods, sample size, and statistical analyses.
• A presentation of the findings in an organized format that helps readers follow along with the author's conclusions.
6. What are common errors in writing literature review?
• Not spending enough time to critically evaluate the relevance of resources, observations and conclusions.
• Totally relying on secondary data while ignoring primary data.
• Letting your personal bias seep into your interpretation of existing literature.
• No detailed explanation of the procedure to discover and identify an appropriate literature review.
7. What are the 5 C's of writing literature review?
• Cite - the sources you utilized and referenced in your research.
• Compare - existing arguments, hypotheses, methodologies, and conclusions found in the knowledge base.
• Contrast - the arguments, topics, methodologies, approaches, and disputes that may be found in the literature.
• Critique - the literature and describe the ideas and opinions you find more convincing and why.
• Connect - the various studies you reviewed in your research.
8. How many sources should a literature review have?
When it is just a chapter, sources should equal the total number of pages in your article's body. if it is a self-contained paper in itself, you need at least three times as many sources as there are pages in your work.
9. Can literature review have diagrams?
• To represent an abstract idea or concept
• To explain the steps of a process or procedure
• To help readers understand the relationships between different concepts
10. How old should sources be in a literature review?
Sources for a literature review should be as current as possible or not older than ten years. The only exception to this rule is if you are reviewing a historical topic and need to use older sources.
11. What are the types of literature review?
• Argumentative review
• Integrative review
• Methodological review
• Systematic review
• Meta-analysis review
• Historical review
• Theoretical review
• Scoping review
• State-of-the-Art review
12. Is a literature review mandatory?
Yes. Literature review is a mandatory part of any research project. It is a critical step in the process that allows you to establish the scope of your research, and provide a background for the rest of your work.
But before you go,
- Six Online Tools for Easy Literature Review
- Evaluating literature review: systematic vs. scoping reviews
- Systematic Approaches to a Successful Literature Review
- Writing Integrative Literature Reviews: Guidelines and Examples
You might also like

Consensus GPT vs. SciSpace GPT: Choose the Best GPT for Research

Literature Review and Theoretical Framework: Understanding the Differences

Types of Essays in Academic Writing - Quick Guide (2024)
Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
- Explore content
- About the journal
- Publish with us
- Sign up for alerts
- CAREER FEATURE
- 04 December 2020
- Correction 09 December 2020
How to write a superb literature review
Andy Tay is a freelance writer based in Singapore.
You can also search for this author in PubMed Google Scholar

Credit: Getty
Literature reviews are important resources for scientists. They provide historical context for a field while offering opinions on its future trajectory. Creating them can provide inspiration for one’s own research, as well as some practice in writing. But few scientists are trained in how to write a review — or in what constitutes an excellent one. Even picking the appropriate software to use can be an involved decision (see ‘Tools and techniques’). So Nature asked editors and working scientists with well-cited reviews for their tips.
WENTING ZHAO: Be focused and avoid jargon
Assistant professor of chemical and biomedical engineering, Nanyang Technological University, Singapore.
When I was a research student, review writing improved my understanding of the history of my field. I also learnt about unmet challenges in the field that triggered ideas.
For example, while writing my first review 1 as a PhD student, I was frustrated by how poorly we understood how cells actively sense, interact with and adapt to nanoparticles used in drug delivery. This experience motivated me to study how the surface properties of nanoparticles can be modified to enhance biological sensing. When I transitioned to my postdoctoral research, this question led me to discover the role of cell-membrane curvature, which led to publications and my current research focus. I wouldn’t have started in this area without writing that review.

Collection: Careers toolkit
A common problem for students writing their first reviews is being overly ambitious. When I wrote mine, I imagined producing a comprehensive summary of every single type of nanomaterial used in biological applications. It ended up becoming a colossal piece of work, with too many papers discussed and without a clear way to categorize them. We published the work in the end, but decided to limit the discussion strictly to nanoparticles for biological sensing, rather than covering how different nanomaterials are used in biology.
My advice to students is to accept that a review is unlike a textbook: it should offer a more focused discussion, and it’s OK to skip some topics so that you do not distract your readers. Students should also consider editorial deadlines, especially for invited reviews: make sure that the review’s scope is not so extensive that it delays the writing.
A good review should also avoid jargon and explain the basic concepts for someone who is new to the field. Although I trained as an engineer, I’m interested in biology, and my research is about developing nanomaterials to manipulate proteins at the cell membrane and how this can affect ageing and cancer. As an ‘outsider’, the reviews that I find most useful for these biological topics are those that speak to me in accessible scientific language.

Bozhi Tian likes to get a variety of perspectives into a review. Credit: Aleksander Prominski
BOZHI TIAN: Have a process and develop your style
Associate professor of chemistry, University of Chicago, Illinois.
In my lab, we start by asking: what is the purpose of this review? My reasons for writing one can include the chance to contribute insights to the scientific community and identify opportunities for my research. I also see review writing as a way to train early-career researchers in soft skills such as project management and leadership. This is especially true for lead authors, because they will learn to work with their co-authors to integrate the various sections into a piece with smooth transitions and no overlaps.
After we have identified the need and purpose of a review article, I will form a team from the researchers in my lab. I try to include students with different areas of expertise, because it is useful to get a variety of perspectives. For example, in the review ‘An atlas of nano-enabled neural interfaces’ 2 , we had authors with backgrounds in biophysics, neuroengineering, neurobiology and materials sciences focusing on different sections of the review.
After this, I will discuss an outline with my team. We go through multiple iterations to make sure that we have scanned the literature sufficiently and do not repeat discussions that have appeared in other reviews. It is also important that the outline is not decided by me alone: students often have fresh ideas that they can bring to the table. Once this is done, we proceed with the writing.
I often remind my students to imagine themselves as ‘artists of science’ and encourage them to develop how they write and present information. Adding more words isn’t always the best way: for example, I enjoy using tables to summarize research progress and suggest future research trajectories. I’ve also considered including short videos in our review papers to highlight key aspects of the work. I think this can increase readership and accessibility because these videos can be easily shared on social-media platforms.
ANKITA ANIRBAN: Timeliness and figures make a huge difference
Editor, Nature Reviews Physics .
One of my roles as a journal editor is to evaluate proposals for reviews. The best proposals are timely and clearly explain why readers should pay attention to the proposed topic.
It is not enough for a review to be a summary of the latest growth in the literature: the most interesting reviews instead provide a discussion about disagreements in the field.

Careers Collection: Publishing
Scientists often centre the story of their primary research papers around their figures — but when it comes to reviews, figures often take a secondary role. In my opinion, review figures are more important than most people think. One of my favourite review-style articles 3 presents a plot bringing together data from multiple research papers (many of which directly contradict each other). This is then used to identify broad trends and suggest underlying mechanisms that could explain all of the different conclusions.
An important role of a review article is to introduce researchers to a field. For this, schematic figures can be useful to illustrate the science being discussed, in much the same way as the first slide of a talk should. That is why, at Nature Reviews, we have in-house illustrators to assist authors. However, simplicity is key, and even without support from professional illustrators, researchers can still make use of many free drawing tools to enhance the value of their review figures.

Yoojin Choi recommends that researchers be open to critiques when writing reviews. Credit: Yoojin Choi
YOOJIN CHOI: Stay updated and be open to suggestions
Research assistant professor, Korea Advanced Institute of Science and Technology, Daejeon.
I started writing the review ‘Biosynthesis of inorganic nanomaterials using microbial cells and bacteriophages’ 4 as a PhD student in 2018. It took me one year to write the first draft because I was working on the review alongside my PhD research and mostly on my own, with support from my adviser. It took a further year to complete the processes of peer review, revision and publication. During this time, many new papers and even competing reviews were published. To provide the most up-to-date and original review, I had to stay abreast of the literature. In my case, I made use of Google Scholar, which I set to send me daily updates of relevant literature based on key words.
Through my review-writing process, I also learnt to be more open to critiques to enhance the value and increase the readership of my work. Initially, my review was focused only on using microbial cells such as bacteria to produce nanomaterials, which was the subject of my PhD research. Bacteria such as these are known as biofactories: that is, organisms that produce biological material which can be modified to produce useful materials, such as magnetic nanoparticles for drug-delivery purposes.

Synchronized editing: the future of collaborative writing
However, when the first peer-review report came back, all three reviewers suggested expanding the review to cover another type of biofactory: bacteriophages. These are essentially viruses that infect bacteria, and they can also produce nanomaterials.
The feedback eventually led me to include a discussion of the differences between the various biofactories (bacteriophages, bacteria, fungi and microalgae) and their advantages and disadvantages. This turned out to be a great addition because it made the review more comprehensive.
Writing the review also led me to an idea about using nanomaterial-modified microorganisms to produce chemicals, which I’m still researching now.
PAULA MARTIN-GONZALEZ: Make good use of technology
PhD student, University of Cambridge, UK.
Just before the coronavirus lockdown, my PhD adviser and I decided to write a literature review discussing the integration of medical imaging with genomics to improve ovarian cancer management.
As I was researching the review, I noticed a trend in which some papers were consistently being cited by many other papers in the field. It was clear to me that those papers must be important, but as a new member of the field of integrated cancer biology, it was difficult to immediately find and read all of these ‘seminal papers’.
That was when I decided to code a small application to make my literature research more efficient. Using my code, users can enter a query, such as ‘ovarian cancer, computer tomography, radiomics’, and the application searches for all relevant literature archived in databases such as PubMed that feature these key words.
The code then identifies the relevant papers and creates a citation graph of all the references cited in the results of the search. The software highlights papers that have many citation relationships with other papers in the search, and could therefore be called seminal papers.
My code has substantially improved how I organize papers and has informed me of key publications and discoveries in my research field: something that would have taken more time and experience in the field otherwise. After I shared my code on GitHub, I received feedback that it can be daunting for researchers who are not used to coding. Consequently, I am hoping to build a more user-friendly interface in a form of a web page, akin to PubMed or Google Scholar, where users can simply input their queries to generate citation graphs.
Tools and techniques
Most reference managers on the market offer similar capabilities when it comes to providing a Microsoft Word plug-in and producing different citation styles. But depending on your working preferences, some might be more suitable than others.
Reference managers
Attribute | EndNote | Mendeley | Zotero | Paperpile |
|---|---|---|---|---|
Cost | A one-time cost of around US$340 but comes with discounts for academics; around $150 for students | Free version available | Free version available | Low and comes with academic discounts |
Level of user support | Extensive user tutorials available; dedicated help desk | Extensive user tutorials available; global network of 5,000 volunteers to advise users | Forum discussions to troubleshoot | Forum discussions to troubleshoot |
Desktop version available for offline use? | Available | Available | Available | Unavailable |
Document storage on cloud | Up to 2 GB (free version) | Up to 2 GB (free version) | Up to 300 MB (free version) | Storage linked to Google Drive |
Compatible with Google Docs? | No | No | Yes | Yes |
Supports collaborative working? | No group working | References can be shared or edited by a maximum of three other users (or more in the paid-for version) | No limit on the number of users | No limit on the number of users |
Here is a comparison of the more popular collaborative writing tools, but there are other options, including Fidus Writer, Manuscript.io, Authorea and Stencila.
Collaborative writing tools
Attribute | Manubot | Overleaf | Google Docs |
|---|---|---|---|
Cost | Free, open source | $15–30 per month, comes with academic discounts | Free, comes with a Google account |
Writing language | Type and write in Markdown* | Type and format in LaTex* | Standard word processor |
Can be used with a mobile device? | No | No | Yes |
References | Bibliographies are built using DOIs, circumventing reference managers | Citation styles can be imported from reference managers | Possible but requires additional referencing tools in a plug-in, such as Paperpile |
*Markdown and LaTex are code-based formatting languages favoured by physicists, mathematicians and computer scientists who code on a regular basis, and less popular in other disciplines such as biology and chemistry.
doi: https://doi.org/10.1038/d41586-020-03422-x
Interviews have been edited for length and clarity.
Updates & Corrections
Correction 09 December 2020 : An earlier version of the tables in this article included some incorrect details about the programs Zotero, Endnote and Manubot. These have now been corrected.
Hsing, I.-M., Xu, Y. & Zhao, W. Electroanalysis 19 , 755–768 (2007).
Article Google Scholar
Ledesma, H. A. et al. Nature Nanotechnol. 14 , 645–657 (2019).
Article PubMed Google Scholar
Brahlek, M., Koirala, N., Bansal, N. & Oh, S. Solid State Commun. 215–216 , 54–62 (2015).
Choi, Y. & Lee, S. Y. Nature Rev. Chem . https://doi.org/10.1038/s41570-020-00221-w (2020).
Download references
Related Articles

- Research management

Why I’ve removed journal titles from the papers on my CV
Career Column 09 AUG 24

Why we quit: how ‘toxic management’ and pandemic pressures fuelled disillusionment in higher education
Career News 08 AUG 24

Scientists are falling victim to deepfake AI video scams — here’s how to fight back
Career Feature 07 AUG 24

Our local research project put us on the global stage — here’s how you can do it, too
Comment 06 AUG 24

Hybrid conferences should be the norm — optimize them so everyone benefits
Editorial 06 AUG 24

How a space physicist is shaking up China’s research funding
News Q&A 02 AUG 24

The UK launched a metascience unit. Will other countries follow suit?
Nature Index 07 AUG 24
Recruitment of Talent Positions at Shengjing Hospital of China Medical University
Call for top experts and scholars in the field of science and technology.
Shenyang, Liaoning, China
Shengjing Hospital of China Medical University
The Recruitment of Fuyao University of Science and Technology
This recruitment of Fuyao University Technologyof Science andUcovers 7 departments including the 6 Schools and the Faculty of Fundamental Disciplines.
Fuzhou, Fujian (CN)
Fuzhou FuYao Institute for Advanced Study
Educational Consultant
You will build and maintain strong relationships with local representatives, key distributors, schools, Ministries of Education, etc.
Riyadh - hybrid working model
Springer Nature Ltd
Senior Marketing Manager – Journal Awareness
Job Title: Senior Marketing Manager – Journal Awareness Location(s): London, UK - Hybrid Working Model Closing date: 25th August 2024 A...
London (Central), London (Greater) (GB)
Faculty Positions& Postdoctoral Research Fellow, School of Optical and Electronic Information, HUST
Job Opportunities: Leading talents, young talents, overseas outstanding young scholars, postdoctoral researchers.
Wuhan, Hubei, China
School of Optical and Electronic Information, Huazhong University of Science and Technology
Sign up for the Nature Briefing newsletter — what matters in science, free to your inbox daily.
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
Reference management. Clean and simple.
Literature review

How to write a literature review in 6 steps
How do you write a good literature review? This step-by-step guide on how to write an excellent literature review covers all aspects of planning and writing literature reviews for academic papers and theses.

How to write a systematic literature review [9 steps]
How do you write a systematic literature review? What types of systematic literature reviews exist and where do you use them? Learn everything you need to know about a systematic literature review in this guide

What is a literature review? [with examples]
Not sure what a literature review is? This guide covers the definition, purpose, and format of a literature review.

Literature Review Example/Sample
Detailed Walkthrough + Free Literature Review Template
If you’re working on a dissertation or thesis and are looking for an example of a strong literature review chapter , you’ve come to the right place.
In this video, we walk you through an A-grade literature review from a dissertation that earned full distinction . We start off by discussing the five core sections of a literature review chapter by unpacking our free literature review template . This includes:
- The literature review opening/ introduction section
- The theoretical framework (or foundation of theory)
- The empirical research
- The research gap
- The closing section
We then progress to the sample literature review (from an A-grade Master’s-level dissertation) to show how these concepts are applied in the literature review chapter. You can access the free resources mentioned in this video below.
PS – If you’re working on a dissertation, be sure to also check out our collection of dissertation and thesis examples here .
FAQ: Literature Review Example
Literature review example: frequently asked questions, is the sample literature review real.
Yes. The literature review example is an extract from a Master’s-level dissertation for an MBA program. It has not been edited in any way.
Can I replicate this literature review for my dissertation?
As we discuss in the video, every literature review will be slightly different, depending on the university’s unique requirements, as well as the nature of the research itself. Therefore, you’ll need to tailor your literature review to suit your specific context.
You can learn more about the basics of writing a literature review here .
Where can I find more examples of literature reviews?
The best place to find more examples of literature review chapters would be within dissertation/thesis databases. These databases include dissertations, theses and research projects that have successfully passed the assessment criteria for the respective university, meaning that you have at least some sort of quality assurance.
The Open Access Thesis Database (OATD) is a good starting point.
How do I get the literature review template?
You can access our free literature review chapter template here .
Is the template really free?
Yes. There is no cost for the template and you are free to use it as you wish.

Psst… there’s more!
This post is an extract from our bestselling short course, Literature Review Bootcamp . If you want to work smart, you don't want to miss this .
What will it take for you to guide me in my Ph.D research work?
Thank you so much for all this information. I am unable to download the literature review template and the excel worksheet. When I click the button it takes me to the top of the page. I would really love to use this template, thank you again!
Submit a Comment Cancel reply
Your email address will not be published. Required fields are marked *
Save my name, email, and website in this browser for the next time I comment.
- Print Friendly

How to Write a Literature Review: Writing a Literature Review in APA Format
- Writing a Literature Review in APA Format
- Chicago/Turabian Citation Style
- Primary and Secondary Sources
- Basic Research Strategies
- Evaluating Sources
- Using the Library's Ebooks
- Using the Library's Catalog
- Copyright Information
- Contact Information & Feedback
Writing a Literature Review in APA
- << Previous: Videos
- Next: APA/Chicago/Turabian/MLA Citation Style >>
- Last Updated: Sep 25, 2023 2:24 PM
- URL: https://tuskegee.libguides.com/c.php?g=692585
How to Write a Literature Review
What is a literature review.
- What Is the Literature
- Writing the Review
A literature review is much more than an annotated bibliography or a list of separate reviews of articles and books. It is a critical, analytical summary and synthesis of the current knowledge of a topic. Thus it should compare and relate different theories, findings, etc, rather than just summarize them individually. In addition, it should have a particular focus or theme to organize the review. It does not have to be an exhaustive account of everything published on the topic, but it should discuss all the significant academic literature and other relevant sources important for that focus.
This is meant to be a general guide to writing a literature review: ways to structure one, what to include, how it supplements other research. For more specific help on writing a review, and especially for help on finding the literature to review, sign up for a Personal Research Session .
The specific organization of a literature review depends on the type and purpose of the review, as well as on the specific field or topic being reviewed. But in general, it is a relatively brief but thorough exploration of past and current work on a topic. Rather than a chronological listing of previous work, though, literature reviews are usually organized thematically, such as different theoretical approaches, methodologies, or specific issues or concepts involved in the topic. A thematic organization makes it much easier to examine contrasting perspectives, theoretical approaches, methodologies, findings, etc, and to analyze the strengths and weaknesses of, and point out any gaps in, previous research. And this is the heart of what a literature review is about. A literature review may offer new interpretations, theoretical approaches, or other ideas; if it is part of a research proposal or report it should demonstrate the relationship of the proposed or reported research to others' work; but whatever else it does, it must provide a critical overview of the current state of research efforts.
Literature reviews are common and very important in the sciences and social sciences. They are less common and have a less important role in the humanities, but they do have a place, especially stand-alone reviews.
Types of Literature Reviews
There are different types of literature reviews, and different purposes for writing a review, but the most common are:
- Stand-alone literature review articles . These provide an overview and analysis of the current state of research on a topic or question. The goal is to evaluate and compare previous research on a topic to provide an analysis of what is currently known, and also to reveal controversies, weaknesses, and gaps in current work, thus pointing to directions for future research. You can find examples published in any number of academic journals, but there is a series of Annual Reviews of *Subject* which are specifically devoted to literature review articles. Writing a stand-alone review is often an effective way to get a good handle on a topic and to develop ideas for your own research program. For example, contrasting theoretical approaches or conflicting interpretations of findings can be the basis of your research project: can you find evidence supporting one interpretation against another, or can you propose an alternative interpretation that overcomes their limitations?
- Part of a research proposal . This could be a proposal for a PhD dissertation, a senior thesis, or a class project. It could also be a submission for a grant. The literature review, by pointing out the current issues and questions concerning a topic, is a crucial part of demonstrating how your proposed research will contribute to the field, and thus of convincing your thesis committee to allow you to pursue the topic of your interest or a funding agency to pay for your research efforts.
- Part of a research report . When you finish your research and write your thesis or paper to present your findings, it should include a literature review to provide the context to which your work is a contribution. Your report, in addition to detailing the methods, results, etc. of your research, should show how your work relates to others' work.
A literature review for a research report is often a revision of the review for a research proposal, which can be a revision of a stand-alone review. Each revision should be a fairly extensive revision. With the increased knowledge of and experience in the topic as you proceed, your understanding of the topic will increase. Thus, you will be in a better position to analyze and critique the literature. In addition, your focus will change as you proceed in your research. Some areas of the literature you initially reviewed will be marginal or irrelevant for your eventual research, and you will need to explore other areas more thoroughly.
Examples of Literature Reviews
See the series of Annual Reviews of *Subject* which are specifically devoted to literature review articles to find many examples of stand-alone literature reviews in the biomedical, physical, and social sciences.
Research report articles vary in how they are organized, but a common general structure is to have sections such as:
- Abstract - Brief summary of the contents of the article
- Introduction - A explanation of the purpose of the study, a statement of the research question(s) the study intends to address
- Literature review - A critical assessment of the work done so far on this topic, to show how the current study relates to what has already been done
- Methods - How the study was carried out (e.g. instruments or equipment, procedures, methods to gather and analyze data)
- Results - What was found in the course of the study
- Discussion - What do the results mean
- Conclusion - State the conclusions and implications of the results, and discuss how it relates to the work reviewed in the literature review; also, point to directions for further work in the area
Here are some articles that illustrate variations on this theme. There is no need to read the entire articles (unless the contents interest you); just quickly browse through to see the sections, and see how each section is introduced and what is contained in them.
The Determinants of Undergraduate Grade Point Average: The Relative Importance of Family Background, High School Resources, and Peer Group Effects , in The Journal of Human Resources , v. 34 no. 2 (Spring 1999), p. 268-293.
This article has a standard breakdown of sections:
- Introduction
- Literature Review
- Some discussion sections
First Encounters of the Bureaucratic Kind: Early Freshman Experiences with a Campus Bureaucracy , in The Journal of Higher Education , v. 67 no. 6 (Nov-Dec 1996), p. 660-691.
This one does not have a section specifically labeled as a "literature review" or "review of the literature," but the first few sections cite a long list of other sources discussing previous research in the area before the authors present their own study they are reporting.
- Next: What Is the Literature >>
- Last Updated: Jan 11, 2024 9:48 AM
- URL: https://libguides.wesleyan.edu/litreview
- UWF Libraries
Literature Review: Conducting & Writing
- Sample Literature Reviews
- Steps for Conducting a Lit Review
- Finding "The Literature"
- Organizing/Writing
- APA Style This link opens in a new window
- Chicago: Notes Bibliography This link opens in a new window
- MLA Style This link opens in a new window
Sample Lit Reviews from Communication Arts
Have an exemplary literature review.
- Literature Review Sample 1
- Literature Review Sample 2
- Literature Review Sample 3
Have you written a stellar literature review you care to share for teaching purposes?
Are you an instructor who has received an exemplary literature review and have permission from the student to post?
Please contact Britt McGowan at [email protected] for inclusion in this guide. All disciplines welcome and encouraged.
- << Previous: MLA Style
- Next: Get Help! >>
- Last Updated: Aug 8, 2024 11:00 AM
- URL: https://libguides.uwf.edu/litreview
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Turk J Urol
- v.39(Suppl 1); 2013 Sep
How to write a review article?
In the medical sciences, the importance of review articles is rising. When clinicians want to update their knowledge and generate guidelines about a topic, they frequently use reviews as a starting point. The value of a review is associated with what has been done, what has been found and how these findings are presented. Before asking ‘how,’ the question of ‘why’ is more important when starting to write a review. The main and fundamental purpose of writing a review is to create a readable synthesis of the best resources available in the literature for an important research question or a current area of research. Although the idea of writing a review is attractive, it is important to spend time identifying the important questions. Good review methods are critical because they provide an unbiased point of view for the reader regarding the current literature. There is a consensus that a review should be written in a systematic fashion, a notion that is usually followed. In a systematic review with a focused question, the research methods must be clearly described. A ‘methodological filter’ is the best method for identifying the best working style for a research question, and this method reduces the workload when surveying the literature. An essential part of the review process is differentiating good research from bad and leaning on the results of the better studies. The ideal way to synthesize studies is to perform a meta-analysis. In conclusion, when writing a review, it is best to clearly focus on fixed ideas, to use a procedural and critical approach to the literature and to express your findings in an attractive way.
The importance of review articles in health sciences is increasing day by day. Clinicians frequently benefit from review articles to update their knowledge in their field of specialization, and use these articles as a starting point for formulating guidelines. [ 1 , 2 ] The institutions which provide financial support for further investigations resort to these reviews to reveal the need for these researches. [ 3 ] As is the case with all other researches, the value of a review article is related to what is achieved, what is found, and the way of communicating this information. A few studies have evaluated the quality of review articles. Murlow evaluated 50 review articles published in 1985, and 1986, and revealed that none of them had complied with clear-cut scientific criteria. [ 4 ] In 1996 an international group that analyzed articles, demonstrated the aspects of review articles, and meta-analyses that had not complied with scientific criteria, and elaborated QUOROM (QUality Of Reporting Of Meta-analyses) statement which focused on meta-analyses of randomized controlled studies. [ 5 ] Later on this guideline was updated, and named as PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses). [ 6 ]
Review articles are divided into 2 categories as narrative, and systematic reviews. Narrative reviews are written in an easily readable format, and allow consideration of the subject matter within a large spectrum. However in a systematic review, a very detailed, and comprehensive literature surveying is performed on the selected topic. [ 7 , 8 ] Since it is a result of a more detailed literature surveying with relatively lesser involvement of author’s bias, systematic reviews are considered as gold standard articles. Systematic reviews can be diivded into qualitative, and quantitative reviews. In both of them detailed literature surveying is performed. However in quantitative reviews, study data are collected, and statistically evaluated (ie. meta-analysis). [ 8 ]
Before inquring for the method of preparation of a review article, it is more logical to investigate the motivation behind writing the review article in question. The fundamental rationale of writing a review article is to make a readable synthesis of the best literature sources on an important research inquiry or a topic. This simple definition of a review article contains the following key elements:
- The question(s) to be dealt with
- Methods used to find out, and select the best quality researches so as to respond to these questions.
- To synthetize available, but quite different researches
For the specification of important questions to be answered, number of literature references to be consulted should be more or less determined. Discussions should be conducted with colleagues in the same area of interest, and time should be reserved for the solution of the problem(s). Though starting to write the review article promptly seems to be very alluring, the time you spend for the determination of important issues won’t be a waste of time. [ 9 ]
The PRISMA statement [ 6 ] elaborated to write a well-designed review articles contains a 27-item checklist ( Table 1 ). It will be reasonable to fulfill the requirements of these items during preparation of a review article or a meta-analysis. Thus preparation of a comprehensible article with a high-quality scientific content can be feasible.
PRISMA statement: A 27-item checklist
| Title | ||
| Title | 1 Identify the article as a systematic review, meta-analysis, or both | |
| Summary | ||
| Structured summary | 2 Write a structured summary including, as applicable, background; objectives; data sources; study eligibility criteria, participants, treatments, study appraisal and synthesis methods; results; limitations; conclusions and implications of key findings; and systematic review registration number | |
| Introduction | ||
| Rationale | 3 Explain the rationale for the review in the context of what is already known | |
| Objectives | 4 Provide an explicit statement of questions being addressed with reference to participants, interventions, comparisons, outcomes, and study design (PICOS) | |
| Methods | ||
| Protocol and registration | 5 Indicate if a review protocol exists, if and where it can be accessed (such as a web address), and, if available, provide registration information including the registration number | |
| Eligibility criteria | 6 Specify study characteristics (such as PICOS, length of follow-up) and report characteristics (such as years considered, language, publication status) used as criteria for eligibility, giving rationale | |
| Sources of Information | 7 Describe all information sources in the survey (such as databases with dates of coverage, contact with study authors to identify additional studies) and date last searched | |
| Survey | 8 Present the full electronic search strategy for at least one major database, including any limits used, such that it could be repeated | |
| Study selection | 9 State the process for selecting studies (that is, for screening, for determining eligibility, for inclusion in the systematic review, and, if applicable, for inclusion in the meta-analysis) | |
| Data collection process | 10 Describe the method of data extraction from reports (such as piloted forms, independently by two reviewers) and any processes for obtaining and confirming data from investigators | |
| Data items | 11 List and define all variables for which data were sought (such as PICOS, funding sources) and any assumptions and simplifications made | |
| Risk of bias in individual studies | 12 Describe methods used for assessing risk of bias in individual studies (including specification of whether this was done at the study or outcome level, or both), and how this information is to be used in any data synthesis | |
| Summary measures | 13 State the principal summary measures (such as risk ratio, difference in means) | |
| Synthesis of outcomes | 14 For each meta-analysis, explain methods of data use, and combination methods of study outcomes, and if done consistency measurements should be indicated (ie P test) | |
| Risk of bias across studies | 15 Specify any assessment of risk of bias that may affect the cumulative evidence (such as publication bias, selective reporting within studies). | |
| Additional analyses | 16 Describe methods of additional analyses (such as sensitivity or subgroup analyses, meta-regression), if done, indicating which were pre-specified. | |
| Results | ||
| Study selection | 17 Give numbers of studies screened, assessed for eligibility, and included in the review, with reasons for exclusions at each stage, ideally with a flow diagram. | |
| Study characteristics | 18 For each study, present characteristics for which data were extracted (such as study size, PICOS, follow-up period) and provide the citation. | |
| Risk of bias within studies | 19 Present data on risk of bias of each study and, if available, any outcome-level assessment (see item 12) | |
| Results of individual studies | 20 For all outcomes considered (benefits and harms), present, for each study, simple summary data for each intervention group and effect estimates and confidence intervals, ideally with a forest plot (a type of graph used in meta-analyses which demonstrates relat, ve success rates of treatment outcomes of multiple scientific studies analyzing the same topic) | |
| Syntheses of resxults | 21 Present the results of each meta-analyses including confidence intervals and measures of consistency | |
| Risk of bias across studies | 22 Present results of any assessment of risk of bias across studies (see item 15). | |
| Additional analyses | 23 Give results of additional analyses, if done such as sensitivity or subgroup analyses, meta-regression (see item 16) | |
| Discussion | ||
| Summary of evidence | 24 Summarize the main findings, including the strength of evidence for each main outcome; consider their relevance to key groups (such as healthcare providers, users, and policy makers) | |
| Limitations | 25 Discuss limitations at study and outcome level (such as risk of bias), and at review level such as incomplete retrieval of identified research, reporting bias | |
| Conclusions | 26 Provide a general interpretation of the results in the context of other evidence, and implications for future research | |
| Funding | ||
| Funding | 27 Indicate sources of funding or other support (such as supply of data) for the systematic review, and the role of funders for the systematic review |
Contents and format
Important differences exist between systematic, and non-systematic reviews which especially arise from methodologies used in the description of the literature sources. A non-systematic review means use of articles collected for years with the recommendations of your colleagues, while systematic review is based on struggles to search for, and find the best possible researches which will respond to the questions predetermined at the start of the review.
Though a consensus has been reached about the systematic design of the review articles, studies revealed that most of them had not been written in a systematic format. McAlister et al. analyzed review articles in 6 medical journals, and disclosed that in less than one fourth of the review articles, methods of description, evaluation or synthesis of evidence had been provided, one third of them had focused on a clinical topic, and only half of them had provided quantitative data about the extend of the potential benefits. [ 10 ]
Use of proper methodologies in review articles is important in that readers assume an objective attitude towards updated information. We can confront two problems while we are using data from researches in order to answer certain questions. Firstly, we can be prejudiced during selection of research articles or these articles might be biased. To minimize this risk, methodologies used in our reviews should allow us to define, and use researches with minimal degree of bias. The second problem is that, most of the researches have been performed with small sample sizes. In statistical methods in meta-analyses, available researches are combined to increase the statistical power of the study. The problematic aspect of a non-systematic review is that our tendency to give biased responses to the questions, in other words we apt to select the studies with known or favourite results, rather than the best quality investigations among them.
As is the case with many research articles, general format of a systematic review on a single subject includes sections of Introduction, Methods, Results, and Discussion ( Table 2 ).
Structure of a systematic review
| Introduction | Presents the problem and certain issues dealt in the review article |
| Methods | Describes research, and evaluation process Specifies the number of studies evaluated orselected |
| Results | Describes the quality, and outcomes of the selected studies |
| Discussion | Summarizes results, limitations, and outcomes of the procedure and research |
Preparation of the review article
Steps, and targets of constructing a good review article are listed in Table 3 . To write a good review article the items in Table 3 should be implemented step by step. [ 11 – 13 ]
Steps of a systematic review
| Formulation of researchable questions | Select answerable questions |
| Disclosure of studies | Databases, and key words |
| Evaluation of its quality | Quality criteria during selection of studies |
| Synthesis | Methods interpretation, and synthesis of outcomes |
The research question
It might be helpful to divide the research question into components. The most prevalently used format for questions related to the treatment is PICO (P - Patient, Problem or Population; I-Intervention; C-appropriate Comparisons, and O-Outcome measures) procedure. For example In female patients (P) with stress urinary incontinence, comparisons (C) between transobturator, and retropubic midurethral tension-free band surgery (I) as for patients’ satisfaction (O).
Finding Studies
In a systematic review on a focused question, methods of investigation used should be clearly specified.
Ideally, research methods, investigated databases, and key words should be described in the final report. Different databases are used dependent on the topic analyzed. In most of the clinical topics, Medline should be surveyed. However searching through Embase and CINAHL can be also appropriate.
While determining appropriate terms for surveying, PICO elements of the issue to be sought may guide the process. Since in general we are interested in more than one outcome, P, and I can be key elements. In this case we should think about synonyms of P, and I elements, and combine them with a conjunction AND.
One method which might alleviate the workload of surveying process is “methodological filter” which aims to find the best investigation method for each research question. A good example of this method can be found in PubMed interface of Medline. The Clinical Queries tool offers empirically developed filters for five different inquiries as guidelines for etiology, diagnosis, treatment, prognosis or clinical prediction.
Evaluation of the Quality of the Study
As an indispensable component of the review process is to discriminate good, and bad quality researches from each other, and the outcomes should be based on better qualified researches, as far as possible. To achieve this goal you should know the best possible evidence for each type of question The first component of the quality is its general planning/design of the study. General planning/design of a cohort study, a case series or normal study demonstrates variations.
A hierarchy of evidence for different research questions is presented in Table 4 . However this hierarchy is only a first step. After you find good quality research articles, you won’t need to read all the rest of other articles which saves you tons of time. [ 14 ]
Determination of levels of evidence based on the type of the research question
| I | Systematic review of Level II studies | Systematic review of Level II studies | Systematic review of Level II studies | Systematic review of Level II studies |
| II | Randomized controlled study | Crross-sectional study in consecutive patients | Initial cohort study | Prospective cohort study |
| III | One of the following: Non-randomized experimental study (ie. controlled pre-, and post-test intervention study) Comparative studies with concurrent control groups (observational study) (ie. cohort study, case-control study) | One of the following: Cross-sectional study in non-consecutive case series; diagnostic case-control study | One of the following: Untreated control group patients in a randomized controlled study, integrated cohort study | One of the following: Retrospective cohort study, case-control study (Note: these are most prevalently used types of etiological studies; for other alternatives, and interventional studies see Level III |
| IV | Case series | Case series | Case series or cohort studies with patients at different stages of their disease states |
Formulating a Synthesis
Rarely all researches arrive at the same conclusion. In this case a solution should be found. However it is risky to make a decision based on the votes of absolute majority. Indeed, a well-performed large scale study, and a weakly designed one are weighed on the same scale. Therefore, ideally a meta-analysis should be performed to solve apparent differences. Ideally, first of all, one should be focused on the largest, and higher quality study, then other studies should be compared with this basic study.
Conclusions
In conclusion, during writing process of a review article, the procedures to be achieved can be indicated as follows: 1) Get rid of fixed ideas, and obsessions from your head, and view the subject from a large perspective. 2) Research articles in the literature should be approached with a methodological, and critical attitude and 3) finally data should be explained in an attractive way.
The Sheridan Libraries
- Write a Literature Review
- Sheridan Libraries
- Evaluate This link opens in a new window
Get Organized
- Lit Review Prep Use this template to help you evaluate your sources, create article summaries for an annotated bibliography, and a synthesis matrix for your lit review outline.
Synthesize your Information
Synthesize: combine separate elements to form a whole.
Synthesis Matrix
A synthesis matrix helps you record the main points of each source and document how sources relate to each other.
After summarizing and evaluating your sources, arrange them in a matrix or use a citation manager to help you see how they relate to each other and apply to each of your themes or variables.
By arranging your sources by theme or variable, you can see how your sources relate to each other, and can start thinking about how you weave them together to create a narrative.
- Step-by-Step Approach
- Example Matrix from NSCU
- Matrix Template
- << Previous: Summarize
- Next: Integrate >>
- Last Updated: Jul 30, 2024 1:42 PM
- URL: https://guides.library.jhu.edu/lit-review

Literature Review Guide: Examples of Literature Reviews
- What is a Literature Review?
- How to start?
- Picking your research question and searching
- Search strategies and Databases
- How to organise the review
- Examples of Literature Reviews
- Library summary
All good quality journal articles will include a small Literature Review after the Introduction paragraph. It may not be called a Literature Review but gives you an idea of how one is created in miniature.
Sample Literature Reviews as part of a articles or Theses
- Hackett, G and Melia, D . The hotel as the holiday/stay destination:trends and innovations. Presented at TRIC Conference, Belfast, Ireland- June 2012 and EuroCHRIE Conference
Links to sample Literature Reviews from other libraries
- Sample literature reviews from University of West Florida

Irish Theses
- Phillips, Martin (2015) European airline performance: a data envelopment analysis with extrapolations based on model outputs. Master of Business Studies thesis, Dublin City University.
- The customers’ perception of servicescape’s influence on their behaviours, in the food retail industry : Dublin Business School 2015
- Coughlan, Ray (2015) What was the role of leadership in the transformation of a failing Irish Insurance business. Masters thesis, Dublin, National College of Ireland.
- << Previous: How to organise the review
- Next: Library summary >>
- Last Updated: Aug 8, 2024 4:32 PM
- URL: https://ait.libguides.com/literaturereview
- Postdoc India
- Postdoc Abroad
- Postdoc (SS)
- RESEARCHERSJOB
- Post a position
- JRF/SRF/Project
- Science News

How to write a literature review: Tips, Format, and Significance

A literature review evaluates available sources on a topic. It analyzes, summarizes, and compares literary works. The review can be included in an article, research report, or thesis, or it can stand alone.
This article provides essential tips on writing a literature review, including format, starting points, common mistakes, and the significance of the literature review. It also discusses how to write a literature review in a step-by-step and pointwise manner.
The literature review typically follows a conventional essay format, consisting of an introduction, body, and conclusion. It differs from a footnoted bibliography, which is a list of resources with individual recaps.
Discover the necessary components for the literature review.
The number of resources you need to examine depends on the literature review and your research proficiency.
A comprehensive literature review should be thorough and able to analyze and summarize extensive details from various sources.
Also read- How Can You Increase Your Citations for a Research Paper: Research Tip
Write an Email to Professor: Complete Dos and Don’ts Discussion
What is the purpose and importance of writing a literature review?
A literature review can increase the number of citations you receive, thereby enhancing your research profile. In general, review papers tend to receive more citations than research articles.If you have knowledge in any subject, it is advisable to write a comprehensive literature review that covers all relevant topics in a wise and informative manner.If you have a comprehensive collection of data on a specific research topic, it is recommended to analyze and synthesize them into an informative literature review article.If you do not have access to a lab facility, it may be beneficial to write a literature review. This will allow you to use your time effectively and maintain a consistent research publication schedule.If your thesis contains sufficient data, it may be beneficial to transform it into a comprehensive literature review paper with additional effort.To create a literature review article, incorporate relevant topics into your research that pertain to a specific problem area.
The literature review demonstrates an understanding and analysis of the existing literature on a particular subject, followed by the synthesis of information.Determine the existing content on a specific topic.Here is a summary of the essential principles.Identify important collaborations or recurring patternsAnalyze the strengths and weaknesses.Please identify any areas that have not been covered in the study.Recognize any conflicting proofProvide a comprehensive background for the research conducted in the term paper.Identify your functionThe literature review should focus on identifying and addressing any unresolved issues.
What is the proper way to begin a Literature Review?
Please select a topic for written discussion.Focus specifically on the concerns related to your research study in that area.Identify and gather the appropriate sources.Determine the range of sources required.Create Your OverviewCreate Your Initial DraftRevise and ModifyCreate a literature review in the form of a paper.
What is your task in your literature review?
Examine your task question and criteria sheet to determine what to focus on when looking for information in the literature.
Conduct a thorough literature review to explore existing research on the topic.
What source for literature??
You should utilize a range of academic and literary sources that are reliable, current, and authoritative in order to gather comprehensive and relevant information. These sources may include books, journal articles, reports, government documents, conference papers, and credible websites. The library collection would be a valuable resource to search for your references.
How many resources??
The number of sources required for a literature review varies depending on its purpose and the individual’s level of study. Guidance from a research guide or previous experience can help determine the necessary amount.
Please remember to note down the bibliographic information of your sources.
Remember to record the research title, date, authors’ names, page numbers, and authors, as this will be beneficial for future reference.
Review the literary works Carefully read each source and look for the disagreements presented rather than focusing on the truths. When creating your testimonial, it is important to structure it by including themes and ideas as you begin and revise. It may be helpful to use a matrix, table, or idea map to visually depict and analyze the relationships between the different sources.Analyze the literature you have. It is necessary to review the sources in order to demonstrate a thorough critical analysis.
When using any resource, it is important to ask the following questions: What are the necessary terms and concepts? How relevant is this short article to my specific topic? What are the major connections and patterns? How did the writer organize their points? How reliable and credible is this source? What are the similarities and differences between the sources? Are there any gaps in the literature that need more research?
How to write a successful literature review.
Avoid rushing to write a substantial literature review on the night before the paper is due.Please begin work on it as soon as possible, including a review of the literature.It is important to also focus on limiting your topic.It is advisable to have someone else proofread your paper before making any changes.Proofreading can assist in catching any mistakes that you may have missed, while also helping you improve your paper.When a document is edited by an expert or reviewed by a buddy or family member, it can make a significant difference.It is important to prioritize your time in order to complete your paper by the due date. Many individuals tend to procrastinate when it comes to completing assignments.Make sure to attend to your paper on a daily basis.Please adhere to the guidelines given to you by your instructor.Please use the appropriate citation style and provide the required number of sources.It is important to have confidence in your literature review.Minor errors can have significant consequences when it comes to quality.
How to write a literature review?
A literature review typically consists of an introduction, body, and conclusion, which provide an overview of the topic and present the overall perspective or argument.
What are the characteristics of an effective literature review?
The information provided should be comprehensive enough to cover the topic adequately.The resource should be concise and reliable.It is important to establish a solid foundation for studying the subject.The research inquiry should be addressed along with the theoretical framework.It is important for you determine research studies and theories that support your topic.The writer must adhere to the specified format design.It is important to find a balance between resources for and against a specific aspect or argument.It should be broad and comprehensive enough to provide the necessary information on the subject.The slimness of your research study should eliminate unnecessary details.It is recommended to obtain information from reliable sources.Arranging literature based on the weight of points provided adds more significance and does not necessarily require logical organization.The paper should address the concerns raised in the research study and incorporate the theoretical framework.The sentence must acknowledge research and evidence that supports the topic.The critical term, terminology, and definitions should be specified.In addition, it is necessary to include the definition of acronyms.A solid foundation for your research study topic can be established through a literature review.
What is the structure of a literature review?
The introduction should include a summary of the content that will be covered. Please explain the purpose of writing a testimonial and the significance of the subject. The scope of the testimony will cover various aspects of the issue. The criteria for selecting literature include the sources used and the range of dates. The review follows an organizational pattern.
The introduction should include.
A literature review can achieve either goal. It can provide statistics or another compelling statement to engage the reader and introduce the topic. It can also affirm the importance of studying the subject. Additionally, it can briefly mention previous research that has been conducted. This summarizes the concluding thoughts derived from the testimonials. The research study addresses weaknesses or gaps in order to strengthen understanding and knowledge.
Body paragraphs.
Each body paragraph should address different relevant motifs related to the subject. It is necessary to incorporate multiple evaluated readings into each section to establish a coherent connection between the various resources. It is essential to analyze each source critically to determine their contribution to the themes being researched.
The body may include sections on:Background history. Approaches. There have been previous research studies conducted on the topic. Conventional versus alternative viewpoints. Initial inquiries are being made. Conclusions are being made.
Conclusion.
The verdict should provide a summary of the information.The literature contains both important arrangements and disagreements.There may be potential gaps or areas that require further investigation.Your perspective on the topic is unbiased.Based on the evidence presented in the literature review, the overall styles and ideas seem to exist.Make a connection between the analysis of existing literature and your own research.
This is a checklist for a literature review.
- Have you thoroughly described the function and scope?
- Can you provide a list of appropriate and credible scholarly literary works?
- Have you recorded the bibliographical details of the sources?
- Have you reviewed and evaluated your analyses?
- There are gaps in the literary works and research that have been identified.
- Have various approaches, theories, hypotheses or versions been explored?
- The differing viewpoints were discussed.Did they consist of a concluding statement, introduction, and main body?
- Have you examined the punctuation as well as the grammar?
It is important to include essential points or fill in any missing information. Thank you.
RELATED ARTICLES MORE FROM AUTHOR
How to turn a manuscript rejection into a success story, phd life blog: 17 things you’ll learn as a ph.d. student, phd guide: how do you know if pursuing a phd is a good investment of your time and money, stress management strategy: 20 simple ways that are actually effective, explain your research paper in a simple way with researchersjob, what is the meaning of letter of intent things you should know about.
If I have to present the literature review in presentation form how that can be done One more question while writing the presentation whether vthe text should contain author name Or not
The same way how you present the research paper in presentation (in a conference or oral presentation), you can do for literature review also. But you need to put a comparative table and scheme to make your presentation more understanding. By adding a scheme, table, chart, etc. you can make your presentation more effective.
As I understand writing a presentation means making conference or oral presentation. Yes, you should give the author name in the first slide in your ppt and the same fore conference board.
This is so informing, however when it comes to creating the gap by using your own words, in most cases supervisors authors. How can someone crest a gap using the researchers words after analysing the literature
Thank You.. finding a gap means, if you read more literature for literature review, then you will get information, and there is some gap/possibility in every work. If you can find that, it will help you to make your flow better for effective literature review writing.
LEAVE A REPLY Cancel reply
Save my name, email, and website in this browser for the next time I comment.
Follow us on Instagram @researchersjob_rj
- Terms Of Service
- Privacy Policy
Postdoctoral Associate | Redox Systems Biology | Agoro Lab, USA
Scholarship opportunity: nucleocytoplasmic shuttling, iimcb, poland.

How to Write a Literature Review

As every student knows, writing informative essay and research papers is an integral part of the educational program. You create a thesis, support it using valid sources, and formulate systematic ideas surrounding it. However, not all students know that they will also have to face another type of paper known as a Literature Review in college. Let's take a closer look at this with our custom essay writer .
Literature Review Definition
As this is a less common academic writing type, students often ask: "What is a literature review?" According to the definition, a literature review is a body of work that explores various publications within a specific subject area and sometimes within a set timeframe.
This type of writing requires you to read and analyze various sources that relate to the main subject and present each unique comprehension of the publications. Lastly, a literature review should combine a summary with a synthesis of the documents used. A summary is a brief overview of the important information in the publication; a synthesis is a re-organization of the information that gives the writing a new and unique meaning.
Typically, a literature review is a part of a larger paper, such as a thesis or dissertation. However, you may also be given it as a stand-alone assignment.
The Purpose
The main purpose of a literature review is to summarize and synthesize the ideas created by previous authors without implementing personal opinions or other additional information.
However, a literature review objective is not just to list summaries of sources; rather, it is to notice a central trend or principle in all of the publications. Just like a research paper has a thesis that guides it on rails, a literature review has the main organizing principle (MOP). The goal of this type of academic writing is to identify the MOP and show how it exists in all of your supporting documents.
Why is a literature review important? The value of such work is explained by the following goals it pursues:
- Highlights the significance of the main topic within a specific subject area.
- Demonstrates and explains the background of research for a particular subject matter.
- Helps to find out the key themes, principles, concepts, and researchers that exist within a topic.
- Helps to reveal relationships between existing ideas/studies on a topic.
- Reveals the main points of controversy and gaps within a topic.
- Suggests questions to drive primary research based on previous studies.
Here are some example topics for writing literature reviews:
- Exploring racism in "To Kill a Mockingbird," "The Adventures of Huckleberry Finn," and "Uncle Tom's Cabin."
- Isolationism in "The Catcher in the Rye," "Frankenstein," and "1984"
- Understanding Moral Dilemmas in "Crime and Punishment," "The Scarlet Letter," and "The Lifeboat"
- Corruption of Power in "Macbeth," "All the King's Men," and "Animal Farm"
- Emotional and Physical survival in "Lord of the Flies," "Hatchet," and "Congo."
How Long Is a Literature Review?
When facing the need to write a literature review, students tend to wonder, "how long should a literature review be?" In some cases, the length of your paper's body may be determined by your instructor. Be sure to read the guidelines carefully to learn what is expected from you.
Keeping your literature review around 15-30% of your entire paper is recommended if you haven't been provided with specific guidelines. To give you a rough idea, that is about 2-3 pages for a 15-page paper. In case you are writing a literature review as a stand-alone assignment, its length should be specified in the instructions provided.
Literature Review Format: APA, MLA, and Chicago
The essay format you use should adhere to the citation style preferred by your instructor. Seek clarification from your instructor for several other components as well to establish a desired literature review format:
- How many sources should you review, and what kind of sources should they be (published materials, journal articles, or websites)?
- What format should you use to cite the sources?
- How long should the review be?
- Should your review consist of a summary, synthesis, or a personal critique?
- Should your review include subheadings or background information for your sources?
If you want to format your paper in APA style, then follow these rules:
- Use 1-inch page margins.
- Unless provided with other instructions, use double-spacing throughout the whole text.
- Make sure you choose a readable font. The preferred font for APA papers is Times New Roman set to 12-point size.
- Include a header at the top of every page (in capital letters). The page header must be a shortened version of your essay title and limited to 50 characters, including spacing and punctuation.
- Put page numbers in the upper right corner of every page.
- When shaping your literature review outline in APA, don't forget to include a title page. This page should include the paper's name, the author's name, and the institutional affiliation. Your title must be typed with upper and lowercase letters and centered in the upper part of the page; use no more than 12 words, and avoid using abbreviations and useless words.
For MLA style text, apply the following guidelines:
- Double your spacing across the entire paper.
- Set ½-inch indents for each new paragraph.
- The preferred font for MLA papers is Times New Roman set to 12-point size.
- Include a header at the top of your paper's first page or on the title page (note that MLA style does not require you to have a title page, but you are allowed to decide to include one). A header in this format should include your full name; the name of your instructor; the name of the class, course, or section number; and the due date of the assignment.
- Include a running head in the top right corner of each page in your paper. Place it one inch from the page's right margin and half an inch from the top margin. Only include your last name and the page number separated by a space in the running head. Do not put the abbreviation p. before page numbers.
Finally, if you are required to write a literature review in Chicago style, here are the key rules to follow:
- Set page margins to no less than 1 inch.
- Use double spacing across the entire text, except when it comes to table titles, figure captions, notes, blockquotes, and entries within the bibliography or References.
- Do not put spaces between paragraphs.
- Make sure you choose a clear and easily-readable font. The preferred fonts for Chicago papers are Times New Roman and Courier, set to no less than 10-point size, but preferably to 12-point size.
- A cover (title) page should include your full name, class information, and the date. Center the cover page and place it one-third below the top of the page.
- Place page numbers in the upper right corner of each page, including the cover page.
Read also about harvard format - popular style used in papers.
Structure of a Literature Review
How to structure a literature review: Like many other types of academic writing, a literature review follows a typical intro-body-conclusion style with 5 paragraphs overall. Now, let’s look at each component of the basic literature review structure in detail:

- Introduction
You should direct your reader(s) towards the MOP (main organizing principle). This means that your information must start from a broad perspective and gradually narrow down until it reaches your focal point.
Start by presenting your general concept (Corruption, for example). After the initial presentation, narrow your introduction's focus towards the MOP by mentioning the criteria you used to select the literature sources you have chosen (Macbeth, All the King's Men, and Animal Farm). Finally, the introduction will end with the presentation of your MOP that should directly link it to all three literature sources.
Body Paragraphs
Generally, each body paragraph will focus on a specific source of literature laid out in the essay's introduction. As each source has its own frame of reference for the MOP, it is crucial to structure the review in the most logically consistent way possible. This means the writing should be structured chronologically, thematically or methodologically.
Chronologically
Breaking down your sources based on their publication date is a solid way to keep a correct historical timeline. If applied properly, it can present the development of a certain concept over time and provide examples in the form of literature. However, sometimes there are better alternatives we can use to structure the body.
Thematically
Instead of taking the "timeline approach," another option can be looking at the link between your MOP and your sources. Sometimes, the main idea will just glare from a piece of literature. Other times, the author may have to seek examples to prove their point. An experienced writer will usually present their sources by order of strength. For example, in "To Kill A Mockingbird," the entire novel was centralized around racism; in "The Adventures of Huckleberry Finn," racism was one of many themes.
Methodologically
As made obvious by the terminology, this type of structuring focuses on the methods used to present the central concept. For example, in "1984", George Orwell uses the law-and-order approach and shows the dangers of a dystopia for a social species.
In "Frankenstein," Mary Shelley exposes the character's physical traits as repulsive and horrifying, forcing him to suffer in an isolated environment. By showcasing the various methods used to portray the MOP, the writer can compare them based on things like severity, ethicality, and overall impact.
After presenting your key findings in the body paragraphs, there are 3 final objectives to complete in the essay's conclusion. First, the author should summarize the findings they have made or found, in other words, and briefly answer the question: "What have you learned?"
After discussing that information, the next step is to present the significance of the information about our current world today. In other words, how can the reader take the information and apply it to today's society? From that point, we finish off with a breadcrumb trail.
As the author, you want to leave the readers' trail of thought within the actual essay topic. This provides them with a means of further investigation—meaning that the reader may consider where the discussion will go next.
Writing an Outline for a Literature Review
Students often underestimate the importance of planning the structure of their papers in advance. However, this is not a wise approach. Having a rough APA literature review outline (or other style outlines) will not only help you follow the right format and structure but will also make the writing process simpler and help ensure that you include all of the important information without missing anything.
How to write a literature review outline: As you already know from the Structure section of this guide, every part of your literature review performs its own important role. Therefore, you should create your outline while keeping the general introduction-body-conclusion structure in mind and ensuring that each section meets its own objectives. However, it is important to remember that a literature review outline is slightly different from outlines of other types of essays because it does not provide new information. Instead, it focuses on existing studies relevant to the main topic.
Here is a literature review outline example on the subject of the Ebola virus to help you get it right:
- Introduce the general topic. Provide background information on the Ebola virus: genome, pathogenesis, transmission, epidemiology, treatment, etc.
- Shape the main research question: What is the potential role of arthropods (mechanical or biological vectors) in the distribution of the Ebola virus?
- Methodology: For example, the information was searched through X databases to find relevant research articles about the Ebola virus and arthropods' role in its spreading. The data was extracted using a standardized form.
- Expected outcomes
- Overall trends in the literature on this topic: While the natural reservoir of the virus is still not known with certainty, many researchers believe that arthropods (and fruit bats, in particular) pay a significant role in the distribution of the virus.
- Subject 1: A brief overview of the particular piece of literature in general terms; an analysis of the key aspects of the study; a review of the research questions, methods, procedures, and outcomes; and an overview of the strong and weak points, gaps, and contradictions.
- Subject 2: A brief overview of the particular piece of literature in general terms; an analysis of the key aspects of the study; a review of the research questions, methods, procedures, and outcomes; and an overview of the strong and weak points, gaps, and contradictions.
- Subject 3: A brief overview of the particular piece of literature in general terms; an analysis of the key aspects of the study; a review of the research questions, methods, procedures, and outcomes; and an overview of the strong and weak points, gaps, and contradictions.
- Indicate the relationships between the pieces of literature discussed. Emphasize key themes, common patterns, and trends. Talk about the pros and cons of the different approaches taken by the authors/researchers.
- State which studies seem to be the most influential.
- Emphasize the major contradictions and points of disagreement. Define the gaps still to be covered (if any).
- If applicable: define how your own study will contribute to further disclosure of the topic.
Hopefully, this sample outline will help you to structure your own paper. However, if you feel like you need some more advice on how to organize your review, don’t hesitate to search for more literature review outline examples in APA or other styles on the Web, or simply ask our writers to get a dissertation help .
Need Help With LITERATURE REVIEW?
Count on our literature review writing service to get it done! We will make your literature essay, we only need your paper requirements to save your precious time and nerves from writing it on your own!
How to Write a Good Literature Review
Whether you are writing a literature review within the framework of a large research project (e.g. thesis, dissertation, or other) or as a stand-alone assignment, the approach you should take to writing generally remains the same.

Whether you are writing a literature review within the framework of a large research project (e.g., thesis, dissertation, or other) or as a stand-alone assignment, the approach you should take to writing generally remains the same.
Now, as you know about the general rules and have a basic literature review outline template, let's define the steps to take to handle this task right with our service:
Step 1: Identifying the Topic
This is probably the only matter you may approach differently depending on whether your literature review comes within a research paper or a separate assignment altogether. If you are creating a literature review as a part of another work, you need to search for literature related to your main research questions and problems. Respectively, if you are writing it as a stand-alone task, you will have to pick a relevant topic and central question upon which you will collect the literature. Earlier in this guide, we suggested some engaging topics to guide your search.
Step 2: Conducting Research
When you have a clearly defined topic, it is time to start collecting literature for your review. We recommend starting by compiling a list of relevant keywords related to your central question—to make the entire research process much simpler and help you find relevant publications faster.
When you have a list of keywords, use them to search for valid and relevant sources. At this point, be sure to use only trusted sources, such as ones from university libraries, online scientific databases, etc.
Once you have found some sources, be sure to define whether or not they are actually relevant to your topic and research question. To save time, you can read abstracts to get general ideas of what the papers are about instead of the whole thing.
Pro Tip: When you finally find a few valid publications, take a look at their bibliographies to discover other relevant sources as well.
Step 3: Assess and Prioritize Sources
Throughout your research, you will likely find plenty of relevant literature to include in your literature review. At this point, students often make the mistake of trying to fit all the collected sources into their reviews. Instead, we suggest looking at what you've collected once more, evaluating the available sources, and selecting the most relevant ones. You most likely won't be able to read everything you find on a given topic and then be able to synthesize all of the sources into a single literature review. That's why prioritizing them is important.
To evaluate which sources are worth including in your review, keep in mind the following criteria:
- Credibility;
- Innovation;
- Key insights;
Furthermore, as you read the sources, don’t forget to take notes on everything you can incorporate into the review later. And be sure to get your citations in place early on. If you cite the selected sources at the initial stage, you will find it easier to create your annotated bibliography later on.
Step 4: Identify Relationships, Key Ideas, and Gaps
Before you can move on to outlining and writing your literature review, the final step is determining the relationships between the studies that already exist. Identifying the relationships will help you organize the existing knowledge, build a solid literature outline, and (if necessary) indicate your own research contribution to a specific field.
Some of the key points to keep an eye out for are:
- Main themes;
- Contradictions and debates;
- Influential studies or theories;
- Trends and patterns;
Here are a few examples: Common trends may include a focus on specific groups of people across different studies. Most researchers may have increased interest in certain aspects of the topic regarding key themes. Contradictions may include some disagreement concerning the theories and outcomes of a study. And finally, gaps most often refer to a lack of research on certain aspects of a topic.
Step 5: Make an Outline
Although students tend to neglect this stage, outlining is one of the most important steps in writing every academic paper. This is the easiest way to organize the body of your text and ensure that you haven't missed anything important. Besides, having a rough idea of what you will write about in the paper will help you get it right faster and more easily. Earlier in this guide, we already discussed the basic structure of a literature review and gave you an example of a good outline. At this workflow stage, you can use all of the knowledge you've gained from us to build your own outline.
Step 6: Move on to Writing
Having found and created all of your sources, notes, citations, and a detailed outline, you can finally get to the writing part of the process. At this stage, all you need to do is follow the plan you've created and keep in mind the overall structure and format defined in your professor's instructions.
Step 7: Adding the Final Touches
Most students make a common mistake and skip the final stage of the process, which includes proofreading and editing. We recommend taking enough time for these steps to ensure that your work will be worth the highest score. Do not underestimate the importance of proofreading and editing, and allocate enough time for these steps.
Pro Tip: Before moving on to proofreading and editing, be sure to set your literature review aside for a day or two. This will give you a chance to take your mind off it and then get back to proofreading with a fresh perspective. This tip will ensure that you won't miss out on any gaps or errors that might be present in your text.
These steps will help you create a top-notch literature review with ease! Want to get more advice on how to handle this body of work? Here are the top 3 tips you need to keep in mind when writing a literature review:
1. Good Sources
When working on a literature review, the most important thing any writer should remember is to find the best possible sources for their MOP. This means that you should select and filter through about 5-10 different options while doing initial research.
The stronger a piece of literature showcases the central point, the better the quality of the entire review.
2. Synthesize The Literature
Make sure to structure the review in the most effective way possible, whether it be chronologically, thematically, or methodologically. Understand what exactly you would like to say, and structure the source comparison accordingly.
3. Avoid Generalizations
Remember that each piece of literature will approach the MOP from a different angle. As the author, make sure to present the contrasts in approaches clearly and don't include general statements that offer no value.
Literature Review Examples
You can find two well-written literature reviews by the EssayPro writing team below. They will help you understand what the final product of a literature review should ideally look like.
The first literature review compares monolingual and bilingual language acquisition skills and uses various sources to prove its point:
The second literature review compares the impact of fear and pain on a protagonist’s overall development in various settings:
Both reviews will help you sharpen your skills and provide good guidelines for writing high-quality papers.
Get Help from an Essay Writer
Still aren’t sure whether you can handle literature review writing on your own? No worries because you can pay for essay writing and our service has got you covered! Boost your grades is to place an order in a few quick clicks and we will satisfy your write my paper request.

is an expert in nursing and healthcare, with a strong background in history, law, and literature. Holding advanced degrees in nursing and public health, his analytical approach and comprehensive knowledge help students navigate complex topics. On EssayPro blog, Adam provides insightful articles on everything from historical analysis to the intricacies of healthcare policies. In his downtime, he enjoys historical documentaries and volunteering at local clinics.


Journals, books & databases
- Author & reviewer hub
- Author guidelines & information
- Prepare your article
Article types

Please note, these guidelines are relevant to all of our journals. Make sure that you check your chosen journal’s web pages for specific guidelines too.
Articles commonly fall into one of three main categories: Full papers, Communications and Reviews. However, each journal will have further, specific article types, so you should always refer to a journal’s specific guidelines while preparing your manuscript.
Full papers are original, unpublished primary research. Extensions of work that has been published previously in short form such as a Communication are usually acceptable.
Communications must contain original and highly significant work whose high novelty warrants rapid publication. Some journals have page limits for Communications.
Reviews may be an authoritative overview of a field, a comprehensive literature review, or tutorial-style reference materials. Reviews are usually invited by the editor, but a topic may be proposed by an author by contacting a journal’s editorial office.
← View all guidelines for preparing and formatting your article
← Explore all information and guidelines for authors
Click through the PLOS taxonomy to find articles in your field.
For more information about PLOS Subject Areas, click here .
Loading metrics
Open Access
Peer-reviewed
Research Article
Knowledge and attitude towards mpox: Systematic review and meta-analysis
Roles Conceptualization, Data curation, Formal analysis, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing
Affiliation Facultad de Medicina Humana, Universidad de San Martín de Porres, Chiclayo, Peru
Roles Conceptualization, Data curation, Investigation, Methodology, Resources, Visualization, Writing – original draft, Writing – review & editing
Affiliation Facultad de Ciencias de la Salud, Escuela de Medicina, Universidad César Vallejo, Trujillo, Peru
Roles Conceptualization, Formal analysis, Investigation, Methodology, Supervision, Visualization, Writing – original draft, Writing – review & editing
Affiliation Faculty of Pharmacy, Mansoura University, Mansoura, Egypt
Roles Conceptualization, Data curation, Formal analysis, Investigation, Methodology, Supervision, Validation, Writing – original draft, Writing – review & editing
Affiliations Department of Microbiology, Tribhuvan University Teaching Hospital, Institute of Medicine, Kathmandu, Nepal, Department of Microbiology, Dr. D. Y. Patil Medical College, Hospital and Research Centre, Dr. D. Y. Patil Vidyapeeth, Pune, Maharashtra, India, Department of Public Health Dentistry, Dr. D.Y. Patil Dental College and Hospital, Dr. D.Y. Patil Vidyapeeth, Pune, Maharashtra, India
* E-mail: [email protected]
Affiliations Universidad Continental, Lima, Peru, Oficina de Epidemiología, Hospital Regional Lambayeque, Chiclayo, Peru
Roles Conceptualization, Data curation, Investigation, Methodology, Project administration, Resources, Supervision, Visualization, Writing – original draft, Writing – review & editing
Affiliations Master of Clinical Epidemiology and Biostatistics, Universidad Cientifica del Sur, Lima, Peru, Gilbert and Rose-Marie Chagoury School of Medicine, Lebanese American University, Beirut, Lebanon
- Darwin A. León-Figueroa,
- Joshuan J. Barboza,
- Abdelmonem Siddiq,
- Ranjit Sah,
- Mario J. Valladares-Garrido,
- Alfonso J. Rodriguez-Morales

- Published: August 9, 2024
- https://doi.org/10.1371/journal.pone.0308478
- Peer Review
- Reader Comments
The increase in mpox incidence underscores the crucial need to understand and effectively address prevention, early detection, and agile response to this disease. Therefore, the present study aims to determine the knowledge and attitude towards mpox.
A systematic review and comprehensive literature meta-analysis were conducted using prominent databases such as PubMed, Scopus, Web of Science, Embase, and ScienceDirect, with an updated search until June 25, 2023. The quality of the included observational studies was assessed using the Joanna Briggs Institute’s Statistical Meta-Analysis Review Instrument. The collected data were recorded in a Microsoft Excel spreadsheet, and analyses were conducted using R software version 4.2.3. Additionally, Cochran’s Q statistics were applied to assess the heterogeneity of the included studies.
A total of 299 articles were retrieved from 5 databases. This study included 27 cross-sectional articles with a total sample of 22,327 participants, of which 57.13% were women. The studies were conducted in 15 countries through an online survey. All studies had a moderate level of quality. The combined prevalence of a good level of knowledge about mpox was 33% (95% CI: 22%-45%; 22,327 participants; 27 studies; I 2 = 100%), and the combined prevalence of a positive attitude towards mpox was 40% (95% CI: 19%-62%; 2,979 participants; 6 studies; I 2 = 99%). Additionally, as a secondary outcome, the combined prevalence of the intention to vaccinate against mpox was 58% (95% CI: 37%-78%; 2,932 participants; 7 studies; I 2 = 99%).
Good knowledge and a positive attitude towards mpox were found to be low. The findings of this study highlight the need to identify gaps and focus on implementing educational programs on mpox.
Joanna Briggs Institute Meta-Analysis of Statistics Assessment and Review Instrument (JBI-MAStARI), Prospective International Registry of Systematic Reviews (PROSPERO), and Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA)
Citation: León-Figueroa DA, Barboza JJ, Siddiq A, Sah R, Valladares-Garrido MJ, Rodriguez-Morales AJ (2024) Knowledge and attitude towards mpox: Systematic review and meta-analysis. PLoS ONE 19(8): e0308478. https://doi.org/10.1371/journal.pone.0308478
Editor: Sirwan Khalid Ahmed, Ministry of Health, General Health Directorate of Raparin and University of Raparin, IRAQ
Received: March 6, 2024; Accepted: July 23, 2024; Published: August 9, 2024
Copyright: © 2024 León-Figueroa et al. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Data Availability: If the data are all contained within the manuscript and/or Supporting Information files, enter the following: All relevant data are within the manuscript and its Supporting Information files.
Funding: The author(s) received no specific funding for this work.
Competing interests: The authors have declared that no competing interests exist.
1. Introduction
The spread of mpox in humans has raised significant concerns in various countries globally, extending beyond Africa, especially in a context marked by the COVID-19 pandemic [ 1 ]. As of June 30, 2024, 97,962 cases of mpox have been reported in 118 countries, 111 of which have not historically reported it [ 2 ].
Mpox is a reemerging zoonotic viral disease caused by the mpox virus, an Orthopoxvirus from the Poxviridae family [ 3 ]. Individuals affected by mpox experience a time interval of 7 to 21 days between exposure and the onset of distinctive clinical symptoms, which include fever, headache, muscle pain, back pain, chills, skin rash, and lymphadenopathy [ 4 ].
The spread of the mpox virus from one person to another extends beyond close direct contact [ 5 ]. Given the rapid development of the mpox virus, how it spreads includes skin wounds, genital lesions, throat secretions, seminal fluid, and blood [ 6 , 7 ]. The rapid expansion of the outbreak in 2022 has raised concerns, mainly because over 95% of the cases affected men who have sex with other men [ 8 , 9 ].
In the face of a public health emergency like the mpox outbreak in 2022, countries must have immediate action plans to prevent diseases promptly. Additionally, providing prevention equipment and disseminating clear information about the signs and symptoms of the disease among the general population is essential [ 10 , 11 ]. It is also vital to ensure that healthcare professionals receive ongoing training or participate in short-term emergency training programs related to mpox [ 10 , 12 ]. These measures will effectively contribute to mitigating the impact of mpox [ 11 ].
Despite efforts and thorough planning, several challenges persist that need to be overcome, including the deficiency in the level of education and the limited knowledge of citizens regarding the current health crisis [ 13 , 14 ]. Therefore, this study aims to determine the combined prevalence of knowledge and attitudes regarding mpox.
2. Materials and methods
2.1. protocol and registration.
This systematic review and meta-analysis were conducted following the guidelines of the PRISMA checklist [ 15 ] ( S1 Table ) . The protocol for this research has been appropriately registered in PROSPERO ( CRD42023439782 ), ensuring transparency and rigor in the process.
2.2. Eligibility criteria
Inclusion criteria..
All observational studies on the prevalence of knowledge, attitude, or both, regarding mpox were considered. No restrictions were imposed regarding gender, health status, language, time, quality, or geographic location. However, only those studies that were available in their entirety provided sample size information presented data related to any aspect of knowledge and attitude towards mpox or provided data from which the required results could be calculated, were included.
Exclusion criteria.
The following studies were excluded: those containing duplicate information, those whose research topics were unrelated to the objective of our study, as well as those using a design different from an observational study. Additionally, articles lacking full text were discarded due to insufficient data or not reporting the desired results.
2.3. Information sources and search strategy
Three expert researchers conducted exhaustive searches in various databases, including PubMed, Scopus, Embase, Web of Science, and ScienceDirect. Keywords such as "mpox," "knowledge," "awareness," and "attitude" were used as part of the search strategy. Specific search strategies for each database are detailed in S2 Table . The initial search was conducted on June 1, 2023, and subsequently updated on June 25, 2023.
2.4. Study selection
The search strategy results were stored and managed using the Endnote software. After eliminating duplicate articles, three experts independently conducted a preliminary selection of the remaining articles by reading the titles and abstracts, following predefined criteria. Subsequently, two other researchers thoroughly reviewed the complete reports to determine if they met the inclusion criteria. Any discrepancies would be resolved through discussions and consultations with a sixth investigator.
2.5. Main and secondary results of the study
This study addressed two main aspects related to knowledge and attitudes towards mpox.
Knowledge about mpox.
The knowledge base of the participants in this study relied on the reports of the included articles, which revealed either good general knowledge or a high level of specific knowledge about mpox. The criteria used to determine the combined prevalence of knowledge covered modes of transmission, clinical symptoms, treatment, prevention, and the diagnosis of mpox.
Attitude towards mpox.
The participants’ attitude in this study was based on the analysis of the included articles, which encouraged a positive attitude towards mpox. Positive attitudes toward mpox included confidence in the overall ability to control the epidemic, in the effectiveness of preventive and control measures, and in the perception that health actions are adequate to prevent its spread.
Intention to vaccinate against mpox.
The intention of the participants to vaccinate against mpox in this study was based on the analysis of the included articles, which reported the importance of getting vaccinated against mpox if the vaccine was available or as a preventive measure.
2.6. Quality assessment
Three independent authors evaluated the quality of the included studies using the "JBI-MAStARI" method for observational studies. In the event of any discrepancies among the evaluators, a fourth author intervened to address and resolve them. To perform this evaluation, a checklist composed of eight critical parameters was used to assess the responses as "yes," "no," "unclear," or "not applicable." The quality of the studies was classified based on their score as high (≥7 points), moderate (4 to 6 points), or low (<4 points) [ 16 ] ( S3 Table ).
2.7. Data collection process and data items
Two independent researchers meticulously collected relevant data from the selected articles. The following details were extracted and recorded in an Excel spreadsheet: first author’s name, publication year, country, sample size, study population, gender (male and female), the prevalence of mpox knowledge, prevalence of attitudes towards mpox, number of cases with knowledge of mpox, and number of cases with attitudes towards mpox. Finally, a third researcher verified the extracted data to ensure accuracy and eliminate incorrect information.
2.8. Data analysis
Firstly, the selected articles were entered into a Microsoft Excel spreadsheet to perform the analysis using R, version 4.2.3. Narrative tables and charts were used to present the research results. To estimate the joint prevalence of mpox knowledge and attitudes, an inverse variance-weighted random-effects model was used. This technique, commonly used in meta-analyses, allows the results of several independent studies to be combined. The model takes into account both within-study variability (within-study variance) and between-study variability (between-study variance) [ 17 ]. The Cochrane Q statistic was employed to assess heterogeneity among studies and quantified using the I 2 index, where 25%, 50%, and 75% indicated low, moderate, and high heterogeneity, respectively [ 18 ]. Funnel plots and Egger’s regression test were used to check for publication bias. Publication bias occurs when the results of published studies are not representative of all studies conducted, usually because studies with non-significant results are less likely to be published [ 19 ]. A possible publication bias was considered when the p-value was < 0.05 [ 20 ].
Subgroup analyses were performed according to study population and country. A forest plot was used to illustrate the combined prevalence of good knowledge and attitudes towards mpox, including 95% confidence intervals.
3.1. Study selection
A total of 299 articles were retrieved from 5 databases. After removing duplicates (n = 125), researchers analyzed 174 articles. Then, the titles and abstracts of these articles were reviewed, and 54 were selected for a thorough full-text review. Finally, 27 articles were included in the study [ 21 – 47 ]. The PRISMA flow diagram shows the study selection process ( Fig 1 ).
- PPT PowerPoint slide
- PNG larger image
- TIFF original image
https://doi.org/10.1371/journal.pone.0308478.g001
3.2. Characteristics of the included studies
This study included 27 cross-sectional articles with a total sample size of 22,327 participants ( Table 1 ). The sample composition consisted of 42.83% males, 57.13% females, and 0.04% others (undefined or unreported) [ 21 – 47 ]. The studies were conducted in 15 countries using an online survey, where questionnaires were sent via e-mail and other communication channels to those with Internet access. The articles cover the period between 2020 and 2023 in their publication year. The sample sizes ranged from 111 to 5,874. Regarding the prevalence of knowledge and attitude towards mpox, the ranges observed were from 0.6% to 65.46% and 12.2% to 84.83%, respectively [ 21 – 47 ].
https://doi.org/10.1371/journal.pone.0308478.t001
3.3. Quality of the included studies and publication bias
The studies were evaluated regarding quality using the JBI-MAStARI for observational research. It was determined that all studies had a moderate level of quality [ 21 – 47 ] ( S3 Table ). We examined the publication bias of articles that reported the level of good knowledge and positive attitude about mpox ( S1 Fig ). Egger’s test, applied to assess publication bias in studies related to the level of good knowledge about mpox, revealed a value of p = 0.0135 (t = 2.66, df = 25), leading to the rejection of the null hypothesis of symmetry. This finding suggests the possible presence of publication bias in the studies analyzed ( S1 Fig ) [ 21 – 47 ]. Articles reporting a positive attitude towards mpox were not assessed for publication bias, as there were fewer than ten studies.
3.4. Level of knowledge of and attitude towards mpox
The aggregated prevalence and 95% confidence interval of knowledge and attitudes towards mpox among study participants are presented in a forest plot ( Figs 2 and 3 ) [ 21 – 47 ]. The random-effects model showed that the combined level of good knowledge about mpox was 33% (95% CI: 22%–45%; 22,327 participants; 27 studies; I 2 = 100%; p < 0.01) ( Fig 2 ) [ 21 – 47 ]. The estimated overall positive attitude towards mpox was 40% (95% CI: 19%–62%; 2,979 participants; 6 studies; I 2 = 99%; p < 0.01) [ 21 , 29 , 32 , 33 , 37 , 43 ] ( Fig 3 ).
https://doi.org/10.1371/journal.pone.0308478.g002
https://doi.org/10.1371/journal.pone.0308478.g003
3.5. Secondary outcomes
The pooled prevalence of intention to vaccinate against mpox was 58% (95% CI: 37%–78%; 2,932 participants; 7 studies; I 2 = 99%; p < 0.01) [ 24 , 30 – 32 , 37 , 43 , 46 ] ( S2 Fig ).
3.6. Subgroup analysis
Subgroup analyses were performed based on the study region and study population [ 21 – 47 ].
3.6.1. Subgroup analysis by study region.
A subgroup analysis was performed based on country. The pooled prevalence of a high level of knowledge about mpox was found to be higher in Algeria (65%, 95% CI: 56%, 74%) [ 31 ] and lower in the Philippines (5%, 95% CI: 3%, 7%) [ 26 ] ( S3 Fig ). However, the pooled prevalence of a positive attitude towards mpox was higher in Bangladesh (85%, 95% CI: 81%, 89%) [ 21 ] and lower in Iraq (12%, 95% CI: 9%, 15%) [ 32 ] ( S4 Fig ).
3.6.2. Subgroup analysis by study population.
A subgroup analysis based on the study population was conducted and divided into two groups: healthcare personnel (doctors, medical students, dental health professionals, and healthcare employees) and the general population (hotel workers, sex workers, university students from different health-related disciplines, and participants from the public). The overall prevalence of a high level of knowledge about mpox was higher in the general population (34%; 95% CI: 23%–46%; 10,505 participants; 12 studies; I 2 = 99%; p < 0.01) [ 23 , 24 , 26 – 28 , 30 , 32 , 34 , 35 , 39 , 41 , 43 ] and lower among healthcare personnel (32%; 95% CI: 17%– 49%; 11,822 participants; 15 studies; I 2 = 100%; p < 0.01) [ 21 , 22 , 25 , 29 , 31 , 33 , 36 – 38 , 40 , 43 – 47 ] ( S5 Fig ). The overall prevalence of a positive attitude towards mpox was higher among healthcare personnel (53%; 95% CI: 26%– 79%; 1,523 participants; 4 studies; I 2 = 99%; p < 0.01) [ 21 , 29 , 33 , 37 ] and lower in the general population (16%; 95% CI: 9%– 25%;1,456 participants; 2 studies; I 2 = 94%; p < 0.01) [ 32 , 43 ] ( S6 Fig ).
4. Discussion
Mpox is not currently considered a public health emergency of international concern; however, it continues to be transmitted in several countries. A thorough understanding of prevention and control measures for this disease is essential.
Given the diversity of research on mpox, multiple studies have been conducted to assess the knowledge of different population targets about mpox to understand the gap of knowledge that can be covered by appropriate educational tools to increase the knowledge score about this disease and to curb its transmission by following the infection control measures [ 21 , 22 , 24 , 48 ]. So we have conducted a systematic review and meta-analysis to gain a more comprehensive understanding of the prevalence of good knowledge levels and attitudes of the general population towards mpox. All relevant studies found through various online search engines were considered to achieve this. Additionally, a subgroup analysis was performed to examine the prevalence of individuals with positive attitudes and a good level of knowledge about mpox based on the region of study and the population analyzed.
The findings of this study revealed that the combined prevalence of good knowledge about mpox was 33%, and the subgroup analysis revealed a total prevalence of good knowledge among the general population and healthcare personnel equal to 34% and 32%, respectively. A meta-analysis by Jahromi AS et al., which included 22 studies involving 27,731 health care workers, revealed that 26% of them had a good knowledge of mpox [ 49 ]. To improve knowledge about mpox, it is crucial to identify reliable and up-to-date sources of information that provide accurate data on its transmission, symptoms, prevention, and treatment. This is essential to effectively understanding and addressing this disease, with a strong emphasis on online sources such as social networks (59%) and the Internet (61%) [ 50 ].
Another result of this study was the combined prevalence of positive attitudes towards mpox, which was 40%. The subgroup analysis results indicated that the combined proportion of positive attitudes towards mpox among healthcare workers was 53%, and the general population was 16%. Different research has assessed this positive attitude towards mpox, ranging from 12% to 85% [ 21 , 29 , 32 , 33 , 37 , 43 ]. A meta-analysis by Jahromi AS et al., which included six studies with 14,388 health care workers, revealed that 34.6% of them had a positive attitude toward mpox [ 49 ]. That could be explained by the disparity in how different populations respond to disease severity and adopt protective measures, which may be attributed to socioeconomic, cultural, information access, and distrust in the healthcare system or government policies. It is essential to address these factors to ensure a more equitable and effective response to any disease and promote the adoption of public health measures to benefit the entire population [ 51 , 52 ].
The difference in the prevalence estimates of the knowledge and the attitude score between our findings and other individual papers may be justified by the difference in the culture of the population from one country to another, the difference in the target group (general population, medical students and healthcare workers), the difference in the timeline at which each study was conducted, the difference in the survey methods used in the assessment of the knowledge and the attitude, and other factors that should be taken into our consideration.
The secondary outcome revealed that the prevalence of the intention to vaccinate against mpox was 58%, consistent with a meta-analysis conducted by Ulloque-Badaracco et al., which reported that the prevalence of mpox vaccine acceptance equals 56% [ 53 ]. Another meta-analysis proposed by León-Figueroa DA et al., which included 29 articles with a total sample of 52,658 participants, determined that the combined prevalence of intention to be vaccinated against mpox was 61% [ 54 ]. It was recommended by the World Health Organization (WHO) and The Center for Disease Control and Prevention (CDC) to vaccinate certain groups of the population who are at risk of developing mpox in terms of pre-exposure and postexposure prophylaxis using JYNNEOS, ACAM2000, and LC16m8 vaccines [ 55 – 57 ]. However, there is variation in the prevalence of intention to vaccinate against mpox reported in the individual studies; this variation could be due to fear of unknown adverse reactions and doubts about the efficacy and safety of the mpox vaccine [ 54 , 58 ].
We recommend that further research is needed to cover the knowledge of the different population groups, including the general public, healthcare professionals, and students, regarding mpox disease, especially in countries with missing data. Further research is needed in countries with many mpox-infected patients at different intervals to track the change in the people’s knowledge, attitude, intention to get vaccinated, and their maintenance on tracking the infection control measures.
This research has several limitations. First, the use of self-reported questionnaires could introduce biases, as participants could provide socially acceptable answers or exaggerate their knowledge about mpox, thus affecting the validity of the data. To mitigate this problem, it is crucial to recommend the use of proxy questions, ensure the anonymity of responses, and perform consistency analysis. Second, the high heterogeneity among the included studies (I 2 > 75%) indicates diversity in the methodologies and populations investigated, which could limit the generalizability of the findings. Our study addressed this issue through subgroup analysis, clear inclusion criteria, and the use of random-effects models, thus providing more accurate and robust data. Third, we found evidence of publication bias, which we addressed using tests such as Egger’s test and funnel plots. Fourth, variations in questionnaire design, distribution methods, and participant demographics could introduce confounding factors into the analysis. Despite these differences, the studies presented similar general criteria regarding transmission, clinical symptoms, diagnosis, treatment, and prevention of mpox. Finally, variability in outcomes could be attributed to sociodemographic, economic, and cultural factors, as well as access to education and trust in the health system or government policies of each country.
Nevertheless, this research has strengths. First, an exhaustive search was carried out in multiple databases without language restrictions, which increased the completeness of the review. Second, robust tools were used to assess quality, and statistical analysis was performed, which reinforced the validity of the results (JBI-MAStARI, PRISMA, Egger’s test, funnel plots, and R software). Third, article selection and data extraction were performed independently by more than three investigators. Finally, this study represents the first systematic review and meta-analysis assessing the prevalence of good knowledge and positive attitudes toward mpox, providing reliable data that can be used by policymakers to improve knowledge and attitudes toward mpox.
5. Conclusions
In conclusion, this systematic review and meta-analysis reported a significant gap in good knowledge and positive attitudes towards mpox. Furthermore, the combined prevalence of good knowledge and positive attitudes differed across study populations, regions, and publication years. A holistic and multisectoral approach is necessary for the successful understanding of mpox. Additional healthcare education and communication are crucial for improving knowledge and attitudes regarding mpox.
Supporting information
S1 table. prisma checklist (prisma 2020 main checklist and primsa abstract checklist)..
https://doi.org/10.1371/journal.pone.0308478.s001
S2 Table. The adjusted search terms as per searched electronic databases.
https://doi.org/10.1371/journal.pone.0308478.s002
S3 Table. Quality of the included studies.
https://doi.org/10.1371/journal.pone.0308478.s003
S1 Fig. Funnel plot and Egger’s test illustrate the publication bias of the included studies.
https://doi.org/10.1371/journal.pone.0308478.s004
S2 Fig. Forest plot showing prevalence of intention to vaccinate against mpox among study participants.
https://doi.org/10.1371/journal.pone.0308478.s005
S3 Fig. Subgroup analysis by country on good knowledge of mpox.
https://doi.org/10.1371/journal.pone.0308478.s006
S4 Fig. Subgroup analysis by country on positive attitude toward mpox.
https://doi.org/10.1371/journal.pone.0308478.s007
S5 Fig. Subgroup analysis by study subjects on good knowledge of mpox.
https://doi.org/10.1371/journal.pone.0308478.s008
S6 Fig. Subgroup analysis by study subjects on positive attitude toward mpox.
https://doi.org/10.1371/journal.pone.0308478.s009
- View Article
- PubMed/NCBI
- Google Scholar
- 2. 2022 Mpox Outbreak Global Map | Mpox | Poxvirus | CDC 2023. https://www.cdc.gov/poxvirus/mpox/response/2022/world-map.html (accessed June 30, 2023).
- 16. JBI Manual for Evidence Synthesis—JBI Global Wiki n.d. https://jbi-global-wiki.refined.site/space/MANUAL (accessed May 15, 2024).
- 17. Chapter 10: Analysing data and undertaking meta-analyses n.d. https://training.cochrane.org/handbook/archive/v6.2/chapter-10 (accessed July 1, 2024).
- 56. Organization WH. Vaccines and immunization for monkeypox: interim guidance, 24 August 2022. World Health Organization; 2022.
- 57. Smallpox/Monkeypox Vaccine Information Statement | CDC 2023. https://www.cdc.gov/vaccines/hcp/vis/vis-statements/smallpox-monkeypox.html (accessed July 30, 2023).
Information
- Author Services
Initiatives
You are accessing a machine-readable page. In order to be human-readable, please install an RSS reader.
All articles published by MDPI are made immediately available worldwide under an open access license. No special permission is required to reuse all or part of the article published by MDPI, including figures and tables. For articles published under an open access Creative Common CC BY license, any part of the article may be reused without permission provided that the original article is clearly cited. For more information, please refer to https://www.mdpi.com/openaccess .
Feature papers represent the most advanced research with significant potential for high impact in the field. A Feature Paper should be a substantial original Article that involves several techniques or approaches, provides an outlook for future research directions and describes possible research applications.
Feature papers are submitted upon individual invitation or recommendation by the scientific editors and must receive positive feedback from the reviewers.
Editor’s Choice articles are based on recommendations by the scientific editors of MDPI journals from around the world. Editors select a small number of articles recently published in the journal that they believe will be particularly interesting to readers, or important in the respective research area. The aim is to provide a snapshot of some of the most exciting work published in the various research areas of the journal.
Original Submission Date Received: .
- Active Journals
- Find a Journal
- Proceedings Series
- For Authors
- For Reviewers
- For Editors
- For Librarians
- For Publishers
- For Societies
- For Conference Organizers
- Open Access Policy
- Institutional Open Access Program
- Special Issues Guidelines
- Editorial Process
- Research and Publication Ethics
- Article Processing Charges
- Testimonials
- Preprints.org
- SciProfiles
- Encyclopedia

Article Menu

- Subscribe SciFeed
- Recommended Articles
- Google Scholar
- on Google Scholar
- Table of Contents
Find support for a specific problem in the support section of our website.
Please let us know what you think of our products and services.
Visit our dedicated information section to learn more about MDPI.
JSmol Viewer
Rhegmatogenous retinal detachment with giant retinal tear: case series and literature review.

1. Introduction
2. materials and methods, 4. discussion, 5. conclusions, author contributions, institutional review board statement, informed consent statement, data availability statement, conflicts of interest.
- Schepens, C.L.; Dobble, J.G.; Mcmeel, J.W. Retinal detachments with giant breaks: Preliminary report. Trans. Am. Acad. Ophthalmol. Otolaryngol. 1962 , 66 , 471–479. [ Google Scholar ]
- Ang, G.S.; Townend, J.; Lois, N. Epidemiology of giant retinal tears in the United Kingdom: The British giant retinal tear epidemiology eye study (BGEES). Retina 2010 , 51 , 4781–4787. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Ghosh, Y.K.; Banerjee, S.; Savant, V.; Kotamarthi, V.; Benson, M.T.; Scott, R.A.; Tyagi, A.K. Surgical treatment and outcome of patients with giant retinal tears. Eye 2004 , 18 , 996–1000. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Shunmugam, M.; Ang, G.S.; Lois, N. Giant retinal tears. Surv. Ophthalmol. 2014 , 59 , 192–216. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Berrocal, M.H.; Chenworth, M.L.; Acaba, L.A. Management of Giant Retinal Tear Detachments. J. Ophthalmic Vis. Res. 2017 , 12 , 93–97. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Kohmoto, R.; Fukumoto, M.; Sato, T.; Oosuka, S.; Kobayashi, T.; Kida, T.; Suzuki, H.; Ikeda, T. Rhegmatogenous retinal detachment with a giant tear located in the intermediate periphery: Two case reports. Medicine 2019 , 98 , e14271. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Samanta, R.; Sood, G.; Waghamare, S.R.; Mareguddi, R.R.; Mittal, S.K.; Agrawal, A. Management of a unique case of post-traumatic posterior giant retinal tear and macular hole-associated rhegmatogenous retinal detachment. Indian J. Ophthalmol. 2020 , 68 , 2577–2580. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Sehgal, P.; Narang, S.; Chandra, D. Rhegmatogenous retinal detachment with giant retinal tear in a child with Marfan’s syndrome: A rare ocular emergency. BMJ Case Rep. 2021 , 14 , e241354. [ Google Scholar ] [ CrossRef ]
- Goezinne, F.; LA Heij, E.C.; Berendschot, T.T.; Gast, S.T.; Liem, A.T.; Lundqvist, I.L.; Hendrikse, F. Low redetachment rate due to encircling scleral buckle in giant retinal tears treated with vitrectomy and silicone oil. Retina 2008 , 28 , 485–492. [ Google Scholar ] [ CrossRef ]
- Leaver, P.K.; Cooling, R.J.; Feretis, E.B.; Lean, J.S.; McLeod, D. Vitrectomy and fluid/ silicone-oil exchange for giant retinal tears: Results at six months. Br. J. Ophthalmol. 1984 , 68 , 432–438. [ Google Scholar ] [ CrossRef ]
- Fan, J.; Lin, J.; Fan, K.C.; Sridhar, J. The Perioperative Management of Giant Retinal Tears. Int. Ophthalmol. Clin. 2020 , 60 , 103–113. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Bottoni, F.; Sborgia, M.; Arpa, P.; De Casa, N.; Bertazzi, E.; Monticelli, M.; De Molfetta, V. Perfluorocarbon liquids as postoperative short-term vitreous substitutes in complicated retinal detachment. Graefes Arch. Clin. Exp. Ophthalmol. 1993 , 231 , 619–628. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Sirimaharaj, M.; Balachandran, C.; Chan, W.C.; Hunyor, A.P.; Chang, A.A.; Gregory-Roberts, J.; Hunyor, A.B.; Playfair, T.J. Vitrectomy with short term postoperative tamponade using perfluorocarbon liquid for giant retinal tears. Br. J. Ophthalmol. 2005 , 89 , 1176–1179. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Ambresin, A.; Wolfensberger, T.J.; Bovey, E.H. Management of giant retinal tears with vitrectomy, internal tamponade, and peripheral 360 degrees retinal photocoagulation. Retina 2003 , 23 , 622–628. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Batman, C.; Cekic, O. Vitrectomy with silicone oil or long-acting gas in eyes with giant retinal tears: Long-term follow-up of a randomized clinical trial. Retina 1999 , 19 , 188–192. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Er, H. Using perfluoro-n-octane as a postoperative tamponade in the management of giant retinal tears. Retina 2006 , 26 , 713. [ Google Scholar ] [ CrossRef ]
- Chang, S.; Lincoff, H.; Zimmerman, N.J.; Fuchs, W. Giant retinal tears. Surgical techniques and results using perfluorocarbon liquids. Arch. Ophthalmol. 1989 , 107 , 761–766. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Nangia, V.; Jonas, J.B.; Sinha, A.; Matin, A.; Kulkarni, M.; Panda-Jonas, S. Ocular Axial Length and Its Associations in an Adult Population of Central Rural India: The Central India Eye and Medical Study. Ophthalmology 2010 , 117 , 1360–1366. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Tideman, J.W.; Snabel, M.C.; Tedja, M.S.; van Rijn, G.A.; Wong, K.T.; Kuijpers, R.W.; Vingerling, J.R.; Hofman, A.; Buitendijk, G.H.; Keunen, J.E.; et al. Association of Axial Length with Risk of Uncorrectable Visual Impairment for Europeans With Myopia. JAMA Ophthalmol. 2016 , 134 , 1355–1363. [ Google Scholar ] [ CrossRef ]
- Kertes, P.J.; Wafapoor, H.; Peyman, G.A.; Calixto, N., Jr.; Thompson, H. The management of giant retinal tears using perfluoroperhydrophenanthrene. A multicenter case series. Vitreon Collaborative Study Group. Ophthalmology 1997 , 104 , 1159–1165. [ Google Scholar ] [ CrossRef ]
- Lee, S.Y.; Ong, S.G.; Wong, D.W.; Ang, C.L. Giant retinal tear management: An Asian experience. Eye 2009 , 23 , 601–605. [ Google Scholar ] [ CrossRef ]
- Fu, Y.; Xie, T.H.; Gu, Z.H.; Yang, N.; Geng, R.F.; Zhang, Y.L. Recurrent retinal detachment after pars plana vitrectomy with silicone oil tamponade for rhegmatogenous retinal detachment. Int. Ophthalmol. 2022 , 42 , 3813–3820. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Bopp, S.; Böhm, K. Reamotio mehr als 1 Jahr nach primär erfolgreicher Ablatiochirurgie: Ursachen und Häufigkeit [Late recurrences more than 1 year after primary successful surgery for rhegmatogenous retinal detachment]. Klin. Monatsblatter Fur Augenheilkd. 2008 , 225 , 227–235. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Quiroz-Reyes, M.A.; Quiroz-Gonzalez, E.A.; Kim-Lee, J.H.; Esparza-Correa, F.; Morales-Navarro, J.G.; Quiroz-Gonzalez, M.A.; Alsaber, A.R.; Moreno-Andrade, B.; Montano, M.; Lima-Gomez, V.; et al. A Critical Analysis of Postoperative Outcomes in Rhegmatogenous Retinal Detachment Associated with Giant Tears: A Consecutive, Multicenter Study. Res. Sq. 2021 , 1 , 1–42. [ Google Scholar ]
- Guner, M.E.; Guner, M.K.; Cebeci, Z.; Kır, N. Preoperative and Postoperative Factors Affecting Functional Success in Anatomically Successful Retinal Detachment Surgery. Korean J. Ophthalmol. 2022 , 36 , 477–485. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Angermann, R.; Bechrakis, N.E.; Rauchegger, T.; Casazza, M.; Nowosielski, Y.; Zehetner, C. Effect of Timing on Visual Outcomes in Fovea-Involving Retinal Detachments Verified by SD-OCT. J. Ophthalmol. 2020 , 2020 , 2307935. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Frings, A.; Markau, N.; Katz, T.; Stemplewitz, B.; Skevas, C.; Druchkiv, V.; Wagenfeld, L. Visual recovery after retinal detachment with macula-off: Is surgery within the first 72 h better than after? Br. J. Ophthalmol. 2016 , 100 , 1466–1469. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Van Bussel, E.M.; van der Valk, R.; Bijlsma, W.R.; La Heij, E.C. Impact of duration of macula-off retinal detachment on visual outcome: A systematic review and meta-analysis of literature. Retina 2014 , 34 , 1917–1925. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Greven, M.A.; Leng, T.; Silva, R.A.; Leung, L.B.; Karth, P.A.; Moshfeghi, D.M.; Sanislo, S.R.; Schachar, I.H. Reductions in final visual acuity occur even within the first 3 days after a macula-off retinal detachment. Br. J. Ophthalmol. 2019 , 103 , 1503–1506. [ Google Scholar ] [ CrossRef ]
- Scott, I.U.; Murray, T.G.; Flynn, H.W., Jr.; Feuer, W.J.; Schiffman, J.C.; Perfluoron Study Group. Outcomes and complications associated with giant retinal tear management using perfluoro-n-octane. Ophthalmology 2002 , 109 , 1828–1833. [ Google Scholar ] [ CrossRef ]
- Aptel, F.; Colin, C.; Kaderli, S.; Deloche, C.; Bron, A.M.; Stewart, M.W.; Chiquet, C.; OSIRIS Group. Management of postoperative inflammation after cataract and complex ocular surgeries: A systematic review and Delphi survey. Br. J. Ophthalmol. 2017 , 101 , 1451–1460. [ Google Scholar ] [ CrossRef ]
- Kim, S.J.; Lo, W.R.; Hubbard, G.B., 3rd; Srivastava, S.K.; Denny, J.P.; Martin, D.F.; Yan, J.; Bergstrom, C.S.; Cribbs, B.E.; Schwent, B.J.; et al. Topical ketorolac in vitreoretinal surgery: A prospective, randomized, placebo-controlled, double-masked trial. Arch. Ophthalmol. 2008 , 126 , 1203–1208. [ Google Scholar ] [ CrossRef ]
- Koerner, F.; Koener-Stiefbold, U.; Garweg, J.G. Systemic corticosteroids reduce the risk of cellophane membranes after retinal detachment surgery: A prospective randomized placebo-controlled double-blind clinical trial. Graefes Arch. Clin. Exp. Ophthalmol. 2012 , 250 , 981–987. [ Google Scholar ] [ CrossRef ]
- Bonfiglio, V.; Reibaldi, M.; Macchi, I.; Fallico, M.; Pizzo, C.; Patane, C.; Russo, A.; Longo, A.; Pizzo, A.; Cillino, G.; et al. Preoperative, Intraoperative and Postoperative Corticosteroid Use as an Adjunctive Treatment for Rhegmatogenous Retinal Detachment. J. Clin. Med. 2020 , 9 , 1556. [ Google Scholar ] [ CrossRef ]
- Nguyen, D.D.; Luo, L.J.; Yang, C.J.; Lai, J.Y. Highly Retina-Permeating and Long-Acting Resveratrol/Metformin Nanotherapeutics for Enhanced Treatment of Macular Degeneration. ACS Nano 2023 , 17 , 168–183. [ Google Scholar ] [ CrossRef ]
- Ting, D.S.W.; Foo, V.H.X.; Tan, T.E.; Sie, N.M.; Wong, C.W.; Tsai, A.S.H.; Tan, G.S.W.; Lim, L.S.; Yeo, I.Y.S.; Wong, D.W.K.; et al. 25-years Trends and Risk factors related to Surgical Outcomes of Giant Retinal Tear-Rhegmatogenous Retinal Detachments. Sci. Rep. 2020 , 10 , 5474. [ Google Scholar ] [ CrossRef ]
Click here to enlarge figure
| Author (Year) | Eyes (n) | Mean Age (Years) | Sex (%) | Etiology | Retinal Reattachment | BCVA 20/40 or Better after OP | Recurrent RD | ||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| M | F | Idiopathic | Trauma | High Myopia | Primary | Final | |||||
| Kertes et al. [ ] (1997) | 162 | N/A | N/A | N/A | N/A | 41 (23.5%) | 20 (12.3%) | 78 (48.1%) | 147 (90.7%) | 24 (14.8%) | 80 (49.4%) |
| Ambresin et al. [ ] (2003) | 18 | 44 | 72 | 28 | N/A | 2 (11.1%) | 7 (38.9%) | 16 (88.9%) | 17 (94.4%) | 9 (50.0%) | 2 (11.1%) |
| Gosh et al. [ ] (2004) | 29 | 35 | 86 | 14 | 10 (34.5%) | 9 (31.0%) | 10 (34.5%) | 19 (65.5%) | 25 (86.2%) | N/A | 6 (20.7%) |
| Sirimaharaj et al. [ ] (2005) | 62 | 44 | 84 | 16 | N/A | 19 (30.6%) | 10 (16.1%) | 49 (79.0%) | 58 (93.5%) | 27 (43.5%) | 13 (21.0%) |
| Goezinne et al. [ ] (2008) | 30 | 53 | N/A | N/A | N/A | 4 (13.3%) | N/A | 21 (70.0%) | 29 (96.7%) | N/A | 9 (30.0%) |
| Lee et al. [ ] (2008) | 128 | 40 | 91 | 9 | N/A | 17 (13.3%) | 52 (40.6%) | 71 (71.7%) | 84 (84.8%) | N/A | 15 (15.2%) |
| Ang et al. [ ] (2010) | 62 | 42 | 72 | 28 | 34 (54.8%) | 10 (16.1%) | 11 (17.7%) | 50 (87.7%) | 54 (94.7%) | 24 (42.1%) | 12 (21.1%) |
| Age | Sex | AXL (mm) | Days to OP | Follow-Up (Months) | BCVA before OP | BCVA after OP | Additional Barrier PC | Complication | |
|---|---|---|---|---|---|---|---|---|---|
| Case 1 | 57 | M | 27.52 | 4 | 6 | 20/100 | 20/20 | 3 | - |
| Case 2 | 66 | M | 23.91 | 0 | 6 | 20/63 | 20/20 | 5 | - |
| Case 3 | 60 | M | 25.98 | 0 | 6 | 20/100 | 20/20 | 0 | Secondary ERM |
| The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
Share and Cite
Lee, S.; Kim, J. Rhegmatogenous Retinal Detachment with Giant Retinal Tear: Case Series and Literature Review. J. Clin. Med. 2024 , 13 , 4690. https://doi.org/10.3390/jcm13164690
Lee S, Kim J. Rhegmatogenous Retinal Detachment with Giant Retinal Tear: Case Series and Literature Review. Journal of Clinical Medicine . 2024; 13(16):4690. https://doi.org/10.3390/jcm13164690
Lee, Siyun, and Joonhyung Kim. 2024. "Rhegmatogenous Retinal Detachment with Giant Retinal Tear: Case Series and Literature Review" Journal of Clinical Medicine 13, no. 16: 4690. https://doi.org/10.3390/jcm13164690
Article Metrics
Article access statistics, further information, mdpi initiatives, follow mdpi.

Subscribe to receive issue release notifications and newsletters from MDPI journals
- Open access
- Published: 06 August 2024
Do behavioral drivers matter for healthcare decision-making during crises? A study of low-income women in El Salvador during the COVID-19 pandemic
- Pedro Bernal Lara 1 ,
- Giuliana Daga 1 ,
- Lajos Kossuth 2 &
- Florencia Lopez Boo 1
BMC Public Health volume 24 , Article number: 2122 ( 2024 ) Cite this article
72 Accesses
Metrics details
Understanding health-seeking behaviors and their drivers is key for governments to manage health policies. A growing body of research explores the role of cognitive biases and heuristics in health and care-seeking behaviors, but little is known about how a context of heightened anxiety and uncertainty might influence these behavioral drivers. This study analyzes the association between four behavioral predictors—internal locus of control, impatience, optimism bias, and aspirations—and healthcare decisions among low-income women in El Salvador, controlling for other factors. We find positive associations between internal locus of control and preventive health behaviors during the COVID-19 pandemic. For instance, a one standard deviation increase in locus of control is associated with a 10% increase in an index measuring the use of masks, distancing, hand washing, and vaccination. Locus of control was also associated with women’s use of preventive health services (one standard deviation improves the likelihood of having a hypertension test in the last six months by 5.8 percentage points). In a sub-sample of mothers, we find significant relationships between the four behavioral drivers and the decisions the mothers make for their children. However, we find these associations are less robust compared to the decisions they make for themselves. Some associations were stronger during the pandemic, suggesting that feelings of uncertainty and stress could amplify behavioral drivers’ influence on health-related behaviors. This novel finding is relevant for designing policy responses for future shocks.
I12, D10, D91, I30.
Peer Review reports
Introduction
Health-seeking decision-making is usually determined by need factors (such as chronic disease status or having a poor health perception) but also by key drivers such as education, health education, income, insurance status, and ability to pay for oneself [ 1 ]. However, healthcare decision-making is so complex that the typical neoclassical economics framework is not sufficient for analyzing it, and we might need to examine factors that go beyond observable variables [ 2 , 3 ]. For instance, people might delay or avoid seeking preventive medical care in the present because they are myopic to the future gains of these interventions [ 4 ]. Others, by being overly optimistic, might underestimate their chances of contracting a disease that is actually seriously contagious [ 5 ].
Less is known about how factors that go beyond observable variables might influence healthcare decision-making in the context of a pandemic, an environment of heightened anxiety and uncertainty. Structural barriers like service disruption significantly influenced how much people utilized healthcare services. In four Latin American countries, service disruptions were associated with increased mortality rates [ 6 ], and in Mexico, they were associated with a decline of over 50% in sick child visits and with a 33% drop in consultations for childhood vaccinations [ 7 ]. However, data limitations made it difficult to disentangle the effect of supply and demand factors. In other developing areas where no restrictions were placed on healthcare services, like rural South Africa, a study found no change in adults’ total daily visits to clinics, but it did find a significant decrease in healthcare visits for children under one year old and one to five years old [ 8 ]. This finding resembles the decrease in children’s healthcare visits in China and children’s vaccination rates in the USA [ 9 , 10 ]. Although the cause is unknown, insufficient childcare options for other children and the fact that these consultations rarely involve medication refills could explain this outcome. Finally, a study using a weekly country-by-county dataset covering the entire Taiwanese population finds that even without taking human mobility restrictions or supply constraints into account, people voluntarily reduced their demand for health care due to fears of contagion or to COVID-related prevention measures [ 11 ].
Researchers have paid less attention to how factors that go beyond structural or observable variables might influence healthcare decision-making during a pandemic. In this context, are people less rational, relying more on heuristics and their cognitive biases to make decisions? Or does the do-or-die nature of the context instead prompt them to prioritize “System 2 thinking,” [ 12 ] which is more rational and deliberate, but is slower and demands more cognitive resources. So far, the evidence on this topic seems mixed in low-income settings or when decisions are made for third parties (like when mothers make decisions on behalf of their children). Some studies have found no discernible differences in economic preferences and decision-making in times of crisis compared to normal times [ 13 ], while others report significant changes in risk tolerance and patience [ 14 , 15 ], stress and depressive symptoms [ 16 ], and internet searches related to economic anxiety, mental health, and well-being [ 17 , 18 , 19 ]. The extent to which behavioral drivers impact decisions during crises could differ by gender. A study using an online sample of 1,500 respondents who were residents of the UK found that women had worse mental health than men and were more pessimistic about the pandemic and economic development [ 20 ].
This article thus explores how behavioral drivers affect healthcare decision-making during a pandemic in a low-income setting in a Central American country. We explore four types of behavioral drivers and their associations with the healthcare decisions of a cross-section of women (and with the healthcare decisions they made for their children in some cases) in low-income communities in El Salvador during the COVID-19 pandemic. Specifically, we rely on survey measures of impatience (how much people value the future versus the present), internal locus of control (the belief that one’s life is contingent on one’s own decisions), optimism bias (the belief that chances of positive events are higher for us than for our peers), and educational aspirations (for the women’s children) which relates to aspirations for the future. We test behavioral drivers’ predictive power by comparing healthcare decisions that were directly related to the COVID-19 pandemic and made during that time with decisions about general healthcare made one year later. The first set of decisions includes compliance with non-pharmaceutical COVID-19 prevention measures (masking, social distancing, and hand washing), COVID-19 vaccination, and avoidance of healthcare services for fear of the pandemic. In their econometric specification, we include restrictions in service supply during 2020 as controls. The second set of decisions includes preventive services for the women, such as screening for chronic conditions (hypertension and diabetes), as well as the use of health and nutrition services—such as prenatal care check-ups and feeding and supplementation practices— for their children.
Several key findings emerge from our analysis. First, locus of control is positively associated with multiple behaviors related to both COVID-19 and general health. For instance, the women’s internal locus of control is positively associated with non-pharmaceutical COVID-19 preventive measures, COVID-19 vaccination, and receiving preventive care services (hypertension check-ups). Interestingly, locus of control has the highest magnitude of correlation with daily behaviors that might be more challenging to adhere to, such as non-pharmaceutical COVID-19 preventive measures. This finding, which as far as we know has not been reported previously in the literature, is not surprising, since those who believe their fate is in their hands will likely take measures to avoid disease in the future.
Second, most behavioral drivers are relevant for non-pharmaceutical COVID-19 preventive measures. In this case impatience, locus of control, and optimism bias are all significant and have a meaningful magnitude of correlation. This is the only outcome for which all three behavioral drivers are jointly significant.
Third, the behavioral drivers of optimism bias and educational aspirations for children are relevant for health service avoidance during the pandemic. Women with higher optimism bias are less likely to have avoided health services for fear of the pandemic, perhaps because they were overconfident that they would not contract COVID-19 while receiving health services. In the same vein, mothers with higher educational aspirations for their children were less likely to avoid healthcare services for their children. This result is probably explained by a positive cost-benefit assessment of the risks of detecting children’s health needs and acting on time, even in the context of a pandemic.
Finally, in line with the literature, people with higher impatience are less likely to engage in healthy behaviors such as non-pharmaceutical COVID-19 prevention measures. These results provide evidence of the relevance of certain behavioral traits in healthcare decision-making during a crisis.
This article is structured as follows. The first section defines the behavioral predictors we use in this study and briefly reviews the literature on those predictors and their relationship with general, health-related decision-making. The second describes the data we used for our estimations. The third presents the econometric specifications and the main results, and the final section contains a brief discussion and a conclusion.
Behavioral drivers and their relevance in the health literature
This section provides a brief overview of the behavioral predictors we use to study healthcare decision-making in the context of the COVID-19 pandemic in El Salvador. We define the predictors and contextualize them within the literature on healthcare decision-making.
Internal locus of control
A person with a high internal locus of control believes that life events are contingent on their own decisions and behaviors instead of other forces like fate or luck [ 21 ]. Several studies have demonstrated a positive relationship between this attribute and different human capital investments, such as educational, job-seeking, and labor market decisions and outcomes [ 22 , 23 , 24 ]. In the health domain, the evidence shows that individuals with a higher internal locus of control prefer to be more present in the decision-making process and take a more active and collaborative role with doctors [ 25 , 26 ]. Likewise, empirical research points to positive associations between higher locus of internal control and healthy living and well-being, and negative associations between this attribute and risky behavior such as tobacco, alcohol, and drug use [ 22 , 27 , 28 ]. People with a high internal locus of control also exhibit better physical and mental health and are less likely to suffer long-term health conditions [ 29 ]. In the field of prenatal and maternal health, a recent study in Nigeria shows that a higher internal locus of control was a significant predictor of utilization of antenatal care and skilled birth care, and of completion of child vaccination [ 30 ]. According to this evidence, people with a higher internal locus of control are more likely to display behaviors related to preventive health.
Impatience measures how much someone values the future relative to the present, and this preference affects inter-temporal decision-making. The literature contains ample evidence of the positive association between patience, human capital investments, and healthy lifestyles [ 31 ]. Further, impatience has been positively associated with obesity [ 32 ], and negatively with preventive health checkups such as fewer mammograms, Pap tests and prostate examinations, dental visits, and flu shot usage [ 4 ]. In sum, more impatient individuals are more likely to make less desirable health-related decisions, since most preventive health investments are realized in the future.
Optimism bias
Optimism bias occurs when people think their chances of experiencing positive events are higher than that of their peers or of the public, or, conversely, that their chances of experiencing negative events are lower [ 33 , 34 ]. A typical example is that most people claim they are less likely than the average driver to be involved in an automobile accident, which is mathematically unfeasible. This behavioral feature is also present in the health domain. People with optimism bias tend to believe they are less likely to experience negative health outcomes [ 35 ], which may hinder efforts to promote preventive, risk-reducing behaviors [ 36 ]. This type of bias is stronger among youth and among people with no active medical symptoms [ 37 ]. . In the context of the pandemic, this bias may help explain why many people refused to wear masks in health facilities and continued to attend large gatherings [ 38 , 39 ]. However, evolutionary models suggest that individuals with optimism bias could be more likely to survive if the benefits of optimism outweigh the cost of inaccurately estimating risk [ 5 , 40 ]. For example, there is a wide body of literature that finds that optimistic individuals were less likely to suffer blood pressure and cardiovascular disease because these people also had increased physical activity and better diet [ 41 , 42 ].
Aspirations
Parents’ aspirations about their children’s future play an important role in overall human capital investments. For example, mothers’ aspirations are important determinants of decisions about their daughters’ schooling [ 43 ] and of their children’s aspirations, achievements, and overall well-being [ 44 ]. Further, parental educational aspirations might lead adolescents to participate in health-promoting activities, like exercise or healthy eating [ 45 ]. According to this evidence, we expect the mothers in our sample with high educational aspirations for their children to behave in ways that promote their children’s health.
Our main data source is a household and facility survey conducted in June 2021 in low-income areas in El Salvador. At that time, the country was rolling out COVID-19 vaccinations, and about one in five people had received at least one dose. Meanwhile, the country was easing restrictions, and COVID-19 cases and mortality had stabilized after the Delta variant surge in January 2021. Footnote 1 The main household survey respondents were women aged 15 to 49, and the questionnaire focused on utilization of health services for them and their children (for those with children younger than 60 months), as well as other health-related behaviors during the COVID-19 pandemic. The survey is unique in that it also includes measures on four behavioral predictors that could be relevant for healthcare decision-making in this context: impatience, internal locus of control, optimism bias, and mothers’ educational aspirations for their own children. In addition to the household survey, we administered a facility survey to the coordinator of the public primary care facility serving women in our sample. Footnote 2 We merged the results from the facility survey with the results from the household survey. Overall, we collected information on 848 women and 60 facilities, which are representative of 14 of the poorest municipalities in El Salvador. Footnote 3 We conducted sampling for the household survey in two stages. We first selected facilities within the 14 municipalities, followed by a random sample of dwellings in the facility’s catchment area to interview women. We interviewed women regardless of whether they received services from the facility.
Main covariates
There are two categories of covariates in our dataset, as shown in Table 1 . Panel A includes individual characteristics of the women and children, as well as proxies for their socioeconomic status. The women in our sample were around 31 years old on average. Most (68.28%) were either married or live in a de facto union, 27.95% have secondary or tertiary education, 57.43% perceive their health to be good, while only around 15% are first-time mothers, and 2.95% live in a household where someone had been diagnosed with COVID-19. Footnote 4 The children in our sample were approximately 1.87 years old on average and were equally distributed by gender. Less than half of them (42.54%) were still breastfed, and their mothers were highly optimistic about their health status. Finally, we use housing conditions (for example, access to electricity, owning a bathroom, type of roof, and floor) and access to treated water as proxies for socioeconomic status. In our sample, only around 21% of households had three or more household assets (i.e., 79% of survey respondents had two or fewer assets), and only 34.67% had access to treated water, which underscores the low-income setting of the population in our sample.
Panel B describes how changes in health service provision during the pandemic affected the women and children in our sample. We find that just under 45% of women live in the catchment area of a facility that suspended health services at some point during 2020. However, child healthcare services were less affected, since only 16% of women experienced a suspension of services. Finally, even though over 35% of women lived in the catchment area of facilities that had staff reductions during 2020, only 4.36% experienced reduced hours. Overall, facilities serving these women had limited shortages of key supplies Footnote 5 (with average shortages of just under two supplies).
Explanatory variables: behavioral predictors
Locus of control.
We use a survey measure of locus of control based on Caliendo et al. (2015) [ 46 ]. Table 2 details the survey questions used for this measure. We find that the population in our sample has an average internal locus of control score of 3.77 out of 5, with 5 being the highest degree of agreement with each statement. The standard deviation for this finding is 0.51. This score means the sample tends to agree more with statements that give themselves a higher degree of responsibility and agency over events. Although we did not find many differences across demographic groups, married women and those who completed high school education or higher have a slightly higher internal locus of control score (Table A S1 ). This finding is partially similar to data from Germany, where married individuals have a lower locus of control and higher educational attainment is associated with higher scores [ 46 ]. The same study also finds that women, immigrants, and older workers have a lower internal locus of control.
Comparing internal locus of control scores with other populations is challenging because of measurement invariance, especially considering the different interpretations of the construct and scales. However, the average in our sample is similar to the averages found in the literature. For instance, a study using a similar instrument to analyze a sample of unemployed individuals in Germany showed a slightly lower score of 3.58 [ 46 ]. Footnote 6 Other locus of control instruments implemented in household surveys in Australia [ 29 ] and Ethiopia [ 47 ] yielded averages that are relatively similar to ours when rescaled to a 5-point scale (3.92 for the former, and 3.45 Footnote 7 for the latter).
We measure impatience according to Falk et al. (2022) [ 48 ]. We ask five questions using the staircase (or unfolding brackets) method, in which subjects choose between a payment today or a larger payment in twelve months. The amount of the hypothetical payment today is the same in each of the situations (10 USD), but the payment in 12 months increases if the respondent answers “today” and decreases if they answer “in 12 months.” All cases assume no inflation, so future prices will be the same as current prices. Each person is scored according to their preferences on a scale of 1 to 32, where 32 is high impatience (we provide a decision-tree with amounts in Appendix Figure A S1 ) We find a very skewed distribution, with a great majority of women in our sample reporting a high level of impatience: 78% of them answered they would prefer to receive 10 USD today, instead of 21.5 USD in 12 months.
We find significant temporal discounting levels, which aligns with previous related research, given the lower-income setting from which the sample was drawn [ 49 ]. Footnote 8 For larger and more heterogeneous populations, previous studies have found that patience is positively associated with higher cognitive ability and varies with age: middle-aged individuals are more patient than young and elderly people. However, we did not found differences by demographic variables (Table A S1 ), probably due to the homogeneity of the sample.
Our survey module on optimism bias measures the women’s degree of confidence about future life events [ 33 ]. The survey questions used for this measure are detailed in Table 3 . This indicator reflects the women’s estimate of how much their chances of experiencing five life events would differ from those of someone with similar characteristics, on a scale of 0 (not likely at all) to 10 (extremely likely). As with the locus of control scale, we inverted questions 2 and 5 to purely measure optimism bias. In general, we find the women in our sample to be overoptimistic. They tend to rate their own likelihood of experiencing a specific life event above the “equally as likely as my neighbor” cutoff for positive events (items 1, 3, and 4), and below and just around it for negative events (items 2 and 5). Concretely, they are optimistic about their economic situation (family having more income next year), and they think they are equally as likely to get robbed as their neighbors. This finding is in line with previous research on automobile accidents, crime, and disease [ 33 , 51 ].
In the health domain, women seem to be relatively overconfident regarding their own health (living longer than 76 years, and not getting sick in the following months) and the health of their children (children growing up healthy and strong). This finding is also in line with the literature on health problems [ 36 ]. Footnote 9 In our sample, married women and women with children are more optimistic, especially with regards to health. In contrast, women with a high school education or higher are less optimistic about health than others with less education (Table A S1 ).
Educational aspirations
We measure educational aspirations as an indicator variable that takes a value of 1 if the mother aspires for their children to achieve a high school education or higher [ 52 ]. Footnote 10 The variable takes a value of 0 if she aspires for her children to complete secondary education or lower, and 1 if her aspirations are for them to partially complete tertiary education or higher. We find that around 73% would like their children to pursue more than a high school education. These percentages are higher than those reported in a rural and poor district in India, where 32% and 18% of parents want their male and female children to graduate from high school [ 52 ], but lower than the 81% of parents in the United States who report in a nationally representative survey in 2012 that they would like their children to complete superior education [ 53 ]. Within our sample, poorer households and women with lower levels of education had lower aspirations for their children (Table A S1 ).
In general, our population shows moderate levels of internal locus of control and high levels of impatience. Table 4 contains descriptive statistics for all our behavioral predictors. Our sample is overly optimistic about general future events, and even more so about health-related events. A majority of women want their children to pursue higher education, although this percentage is low compared to representative samples in industrialized countries. Table A S2 in the appendix shows the positive correlations between internal locus of control and educational aspirations, as well as a weaker correlation between internal locus of control and general optimism bias.
Outcome variables: healthcare decision-making
We classify the outcome variables in our study as either healthcare decision-making related to the COVID-19 pandemic, or what we consider to be general health behaviors (i.e., check-ups, preventive health services, and diet/nutrition, among others). The first category reflects novel behaviors that became relevant during the COVID-19 pandemic, whereas the second category contains usual health behaviors in the population of interest. Table 5 contains descriptive statistics for both types of behavior. In behaviors related to COVID-19 (Panel A of Table 5 ), 6.01% of the women in our sample report having avoided health services for themselves or a household member for fear of contracting COVID-19, while 8.33% of women with children under five years old avoided health services for their children because of that same reason. The average COVID-19 non-pharmaceutical prevention index for women in our sample was 3.05, which indicates that the women complied with at least three prevention measures (whether always using a mask, practicing social distancing, disinfecting their hands, or disinfecting objects around them in the last seven days). Finally, 83.84% of the women said they had been vaccinated against COVID-19 or were willing to be vaccinated.
Panel B of Table 5 shows that in our sample, around 30% of women had their blood pressure taken in the preceding six months and 17% had a blood glucose level test in that same period. This suggests relatively low take-up of these preventive services. Conversely, women with children under age five are extremely compliant with prenatal visits, as almost 90% of them report having gone to at least four during their most recent pregnancy in the last five years. Regarding feeding practices, only 10.45% of mothers gave their children the recommended dosage of micronutrients in the last six months, and, on average, they served only 2.28 out of 6 iron-rich food items in the last day.
Econometric specification and results
To assess the relationship between our four behavioral predictors and the healthcare decisions people make in the context of the COVID-19 pandemic, we estimate a series of analogous OLS regressions. We split up the analysis according to the nature of outcomes. First, we focus on novel healthcare decisions related to the COVID-19 pandemic. Then we analyze general healthcare decisions that are independent of the pandemic (such as using preventive health services). The main specification for these regressions is:
Where \({y}_{ifj}\) is one of our selected health outcomes for respondent i in facility f in municipality j; \({Locus}_{ifj}\) is the internal locus of control measure for respondent i in facility f in municipality j; \({Impatience}_{ifj}\) is the impatience measure for respondent i in facility f in municipality j; \({Optimism bias}_{ifj}\) is the optimism bias measure at the individual level i in facility f in municipality j; \({W}_{ifj}\) are individual controls for women; \({H}_{fj}\) are health services controls; \({\gamma }_{j}\) are municipality fixed effects; and \({\epsilon }_{ifj}\) is the error term. The coefficients of interest are \({\beta }_{1}\) , \({\beta }_{2}\) , and \({\beta }_{3}\) , which measure the degree to which each behavioral predictor is associated with the specific health outcome. For child-specific outcomes, we take a subsample that includes only mothers and modify equation (i) by adding child individual controls, and include a fourth behavioral predictor: \({Aspirations}_{ifj}\) . We use the same base specification for outcomes related to both COVID-19 and general health behaviors, except that we do not include health facility controls for general health behaviors since they have a different time frame: our health facility controls focus on how services were affected during 2020, whereas the reference period for general health behaviors is 2021. We conduct several robustness checks of the results for both sets of outcomes, assessing the individual association between each behavioral driver and outcome (Appendix Tables A3 and A4 ), sensitivity to different specifications (no controls and adding facility fixed effects), to multiple hypothesis testing, and to omitted variable bias (Appendix Tables A S5 and A S6 ), as well as to outliers (Appendix Figures A S2 and A S3 ).
Results for COVID-19-related health behaviors
Our dataset contains the following COVID-19-related outcomes: (i) avoidance of health services (for the women, child, or another household member) for fear of the pandemic; (ii) compliance with COVID-19 non-pharmaceutical prevention measures; and (iii) having been vaccinated against COVID-19 or being willing to be vaccinated. All women in the sample responded the survey items on avoidance of health services for the woman or another household member, vaccination, and compliance with prevention methods. However, only women who are mothers of children between the ages of 0 and 5 responded to the question related to avoidance of health services for the child.
Table 6 presents the results of this first set of estimations. All behavioral predictors (impatience, internal locus of control, optimism bias, and educational aspirations) are standardized with a mean of 0 and standard deviation of 1 to make their association with the outcome variables comparable. We start with impatience. The literature predicts that more impatient individuals tend to adhere less to healthcare guidelines. Indeed, we find that an increase of one standard deviation in impatience is associated with 0.118 fewer points in an index of COVID-19 non-pharmaceutical prevention measures. Internal locus of control, on the other hand, is positively associated with COVID-19 non-pharmaceutical prevention measures, COVID-19 vaccination status, and healthcare avoidance: an increase of one standard deviation in internal locus of control predicts 0.277 more points in an index of COVID-19 preventive behaviors (a 10% increase relative to the mean), a 3.4 percentage points rise in the likelihood of having been vaccinated or being willing to be vaccinated, and a 2 percentage point increase in the likelihood of avoiding health services for fear of the pandemic. These results also align with the predictions in the literature: a higher degree of internal locus of control should be associated with believing that everyone is more in control of their destiny and thus that their health status is mainly their responsibility.
Optimism bias negatively predicts whether a woman or a household member avoided going to a healthcare facility for themselves or their child for fear of COVID-19. Our interpretation of these results is that women were overly optimistic about not contracting COVID-19 during their health visit. If they are biased towards optimism about remaining healthy despite the risk of contracting COVID-19, they might still decide to go to the health center and take care of their health needs. However, optimism bias is at the same time positively associated with compliance with non-pharmaceutical prevention measures. This surprising result might be related to different types of risks and behaviors in response to them. Finally, a mother’s educational aspirations for her children are negatively associated with avoiding health services for her children because of fear of COVID-19. We find that mothers with higher aspirations for their children are 3.2 percentage points less likely to avoid or postpone healthcare services for their children, which is in line with the literature. However, this result is not robust to the inclusion of facility fixed effects, as we lose precision, but the coefficient is still similar in magnitude (Appendix Table A S5 ).
Results for general health behaviors
We use the following general health outcomes as general health behaviors: (i) test for hypertension in the last six months; (ii) test for diabetes in the last six months; (iii) at least four prenatal visits; (iv) children’s consumption of micronutrients in the last six months; and (v) number of iron-rich food items consumed by children. Again, it is worth noting that the number of observations in each regression will depend on the type of outcome, as some apply to all women in the sample and others just to women with children. For example, the entire sample of women responded to the survey items on hypertension and diabetes. In contrast, only women who are mothers of children between the ages of 0 and 5 responded to the child-related outcomes, except for the question related to an iron-rich diet, which was restricted to mothers of children over one year old, where most children have made the transition to solid foods.
Table 7 presents the results of this second set of estimations. We focus on associations that are below the 5% significance level, as those significant at the 10% level are not robust (Appendix Table A S6 ). We observe that impatience negatively predicts feeding children micronutrients on 60 days in a six-month period. Internal locus of control, on the other hand, is positively associated with having been tested for hypertension in the last six months and an increased number of iron-rich food items consumed by children. Notably, an increase of one standard deviation in internal locus of control is associated with an increase of 5.8 percentage points in likelihood of having a hypertension screening. This correlation likely indicates that women who believe their destiny is in their own hands will try to guarantee the best possible health status. Although we find no significant association between internal locus of control and diabetes detection, this may be because the disease is less common than hypertension. Overall, Table 7 shows only weak associations for child-related general behaviors, as these associations are sensitive to our robustness checks (Appendix Table A S6 ), in contrast to the association between locus of control and hypertension screening, which is very strong. It is unclear whether the associations are weak because the behavioral predictors we measured for women do not have explanatory value for mothers’ caregiving behavior or because we have little power to detect them since the child-related sample is smaller. The associations we found were more robust in behaviors related to COVID-19, which suggests that feelings of uncertainty and stress could enhance the predictive power of our chosen behavioral predictor and that they may play an important role in novel behaviors.
Conclusions
Historically, there have been clear socio-economic disparities in decision-making about the utilization of healthcare, which has always been shaped by need factors and observable drivers such as education, income, insurance status, and ability to pay. This study goes beyond traditional determinants and analyzes four types of behavioral predictors—impatience, internal locus of control, optimism bias, and aspirations—and their associations with decisions about healthcare among low-income women in El Salvador in the context of the COVID-19 pandemic.
Our results provide some novel insights. First, we find that our behavioral predictors are more significantly associated with healthcare decisions that are related to the pandemic. For example, impatience and locus of control have higher magnitudes and significance for COVID-19 prevention measurements. Especially salient is the case of optimism bias, which seems to predict less avoidance of health services for fear of the pandemic but exhibits no significant correlations with other decisions related to utilizing general health services. It is possible that the scale and nature of the event enhanced the influence of behavioral predictors on healthcare decisions to the detriment of a more rational approach to decision-making. This hypothesis is worth considering for future shocks like natural disasters, health emergencies, or situations of social unrest.
Second, most of the correlations we found align with what we would have predicted based on theory. Still, additional evidence is needed to support these conclusions, especially in a low-income setting. For instance, resembling previous literature, our study finds that, on average, higher internal locus is associated with healthier behaviors. Likewise, our study finds that women with optimism bias were less likely to avoid attending health facilities for fear of COVID-19, signaling that they were overconfident that they would not contract the disease. Moreover, impatience negatively predicts prevention measures, which denotes the tension between present costs and future health benefits. While these findings are aligned with previous research, this is one of the first studies that analyze these relationships in a low-income setting. Finally, while the behavioral predictors are significant and robust for women’s health behaviors, they are not robust in the subsample of mothers with children. From the available evidence, it is unclear whether the behavioral traits we measured for women are not relevant for health behaviors for their children or just that they have less power to detect them since the sample is smaller.
Our study has some limitations. First, since it is an observational study, we cannot rule out the presence of reverse causality, which can potentially influence the observed relationships between variables. For instance, it is not clear whether having good health might influence some of the behavioral drivers we analyze or vice-versa. Second, the generalizability of our findings may be restricted due to the specific demographic composition of our sample, which is consists exclusively of women from low-income settings. Finally, our survey was conducted in mid-2021, when El Salvador was transitioning out of lockdowns and expanding its coverage of COVID-19 vaccinations. Since this was an atypical time, it is not clear whether our findings for general health behaviors will be the same a few years after the pandemic. These limitations underscore the need for further research using diverse methodologies and broader study populations to validate and extend our findings.
Understanding people’s reasoning processes as they make healthcare decisions is key to improving policy design. Our study aims to expand the evidence on this topic with data from disadvantaged women in a developing country. To the best of our knowledge, it is also among the first to compare healthcare decisions related to the COVID-19 pandemic with those related to general health behaviors. In addition, we contribute to the literature by analyzing how these behavioral predictors affect third parties: the children of some of the women in our sample. Our results emphasize the need for further research that can provide specific strategies informed by behavioral sciences to improve health seeking behaviors and establish causal associations, which is something this study is not able to do. Our findings also shed light on the potentially effective role of behavioral strategies in improving the healthcare-seeking behaviors of the most vulnerable populations, which may have different patterns of locus of control, impatience, optimism, and aspirations than the general population.
Data availability
The datasets supporting the conclusions of this article are available in the IDB Social Data repository ( https://scldata.iadb.org ). It is available from the corresponding author upon reasonable request.
This statement is based on data compiled by the Inter-American Development in a COVID-19 Situational Update report for Latin American and the Caribbean Bank as of June 15, 2021. The report is available at http://www.iadb.org/document.cfm? id=EZSHARE-2024879176-650 .
Public health facilities are the main provider in survey locations. For example, according to UNICEF’s Multiple Indicator Cluster Survey (2014), in 2014, the Ministry of Health provided around 93% of postnatal care services in rural areas, which are the main type of areas captured in our survey.
The survey is representative of women living in 14 municipalities in El Salvador: Chiltiupán, Tacuba, El Sauce, Sociedad, Ilobasco, Sensuntepeque, Monte San Juan, San Cristóbal, San Antonio Masahuat, Santa María Ostuma, Apastepeque, San Esteban Catarina, San Ildefonso, and Tecoluca.
This refers only to self-reported COVID-19 diagnoses of woman or household members by test or health personnel prior to the survey. If someone in a household had COVID-19 at the time of the survey, that household was not included in the sample due to the health security protocol.
Examples of medical supplies include oral hydration salts, zinc, antibiotics for respiratory infections and vaccines (BCG, polio, measles, mumps, rubella, rotavirus, pneumococcal conjugate, or influenza).
Author’s calculation based on the procedure described in the footnote to Table 2 and by converting scores as a proportion of 5 instead of 7, which is the scale used for the study.
This score was calculated by reversing the items associated with external locus of control.
Previous research found that countries with lower incomes usually have greater temporal discounting [ 49 ], although economic inequality and broader financial circumstances are important [ 50 ].
It is possible that health-related optimism varies considerably depending on more specific health-related risks [ 35 ].
We ask mothers: “What is the highest level of completed education you would like for your child to achieve?”
Abuduxike G, Aşut Ö, Vaizoğlu SA, Cali S. Health-seeking behaviors and its determinants: a facility-based cross-sectional study in the Turkish Republic of Northern Cyprus. Int J Health Policy Manag. 2019;1.
Mullainathan S, Thaler RH. Behavioral economics. International Encyclopedia of Social Sciences Vol. 20, 1094–1100. Oxford University Press; 2001.
Frank R. Behavioral economics and health economics, Diamond, Vartiainen, editors, Behavioral Economics and Its Applications. Princeton Univ. Press, Princeton, NJ; 2007.
Bradford WD. The Association between Individual Time Preferences and Health Maintenance habits. Med Decis Mak. 2010;30(1):99–112.
Article Google Scholar
Gassen J, Nowak TJ, Henderson AD, Weaver SP, Baker EJ, Muehlenbein MP. Unrealistic optimism and risk for COVID-19 disease. Front Psychol. 2021;12:647461.
Article PubMed PubMed Central Google Scholar
Bernal Lara P, Savedoff WD, García Agudelo MF, Bernal C, Goyeneche L, Sorio R, et al. Disruption of Non-COVID-19 Health Care in Latin America during the pandemic: effects on Health, lessons for policy: study examines the disruption of non-COVID-19 health care in Latin America. Health Aff. 2023;42(12):1657–66.
Doubova SV, Leslie HH, Kruk ME, Pérez-Cuevas R, Arsenault C. Disruption in essential health services in Mexico during COVID-19: an interrupted time series analysis of health information system data. BMJ Glob Health. 2021;6(9):e006204.
Article PubMed Google Scholar
Siedner MJ, Kraemer JD, Meyer MJ, Harling G, Mngomezulu T, Gabela P, et al. Access to primary healthcare during lockdown measures for COVID-19 in rural South Africa: an interrupted time series analysis. BMJ Open. 2020;10(10):e043763.
Santoli JM. Effects of the COVID-19 Pandemic on Routine Pediatric Vaccine Ordering and Administration — United States, 2020. MMWR Morb Mortal Wkly Rep [Internet]. 2020 [cited 2024 Mar 26];69. https://www.cdc.gov/mmwr/volumes/69/wr/mm6919e2.htm .
Li H, Yu G, Duan H, Fu J, Shu Q. Changes in children’s Healthcare visits during coronavirus Disease-2019 pandemic in Hangzhou, China. J Pediatr. 2020;224:146–9.
Article CAS PubMed PubMed Central Google Scholar
Tsai YY, Yang TT. Measuring voluntary responses in healthcare utilization during the COVID-19 pandemic: Evidence from Taiwan. Rahman MS, editor. PLoS ONE. 2022;17(12):e0271810.
Kahneman D. Thinking, fast and slow. Macmillan. New York; 2011.
Drichoutis AC, Nayga RM Jr. On the stability of risk and time preferences amid the COVID-19 pandemic. Exp Econ. 2022;25(3):759–94.
Aragon FM, Bernal N, Mossi MB, Molina O. COVID-19 and economic preferences: evidence from a panel of cab drivers. Netspar, Network for Studies on Pensions, Aging and Retirement; 2022.
Harrison GW, Hofmeyr A, Kincaid H, Monroe B, Ross D, Schneider M, et al. Subjective beliefs and economic preferences during the COVID-19 pandemic. Exp Econ. 2022;25(3):795–823.
Holman EA, Thompson RR, Garfin DR, Silver RC. The unfolding COVID-19 pandemic: a probability-based, nationally representative study of mental health in the United States. Sci Adv. 2020;6(42):eabd5390.
Fetzer T, Hensel L, Hermle J, Roth C. Coronavirus perceptions and economic anxiety. Rev Econ Stat. 2021;103(5):968–78.
Brodeur A, Clark AE, Fleche S, Powdthavee N. COVID-19, lockdowns and well-being: evidence from Google Trends. J Public Econ. 2021;193:104346.
Silverio-Murillo A, Hoehn-Velasco L, Rodriguez Tirado A, Balmori de la Miyar JR. COVID-19 blues: lockdowns and mental health-related Google searches in Latin America. Soc Sci Med. 2021;281:114040.
Oreffice S, Quintana-Domeque C. Gender inequality in COVID-19 times: evidence from UK prolific participants. J Demographic Econ. 2021;87(2):261–87.
Rotter JB. Generalized expectancies for internal versus external control of reinforcement. Psychol Monographs: Gen Appl. 1966;80(1):1.
Article CAS Google Scholar
Heckman J, Stixrud J, Urzua S. The effects of cognitive and noncognitive abilities on labor market outcomes and social behavior. J Labor Econ. 2006;24(3):411–82.
Caliendo M, Cobb-Clark DA, Obst C, Seitz H, Uhlendorff A. Locus of control and investment in training. J Hum Resour. 2022;57(4):1311–49.
McGee A, McGee P. Search, effort, and locus of control. J Econ Behav Organ. 2016;126:89–101.
Marton G, Pizzoli SFM, Vergani L, Mazzocco K, Monzani D, Bailo L, et al. Patients’ health locus of control and preferences about the role that they want to play in the medical decision-making process. Psychol Health Med. 2021;26(2):260–6.
Nazareth M. Relating Health Locus of Control to Health Care Use, Adherence, and Transition Readiness Among Youths With Chronic Conditions, North Carolina, 2015. Prev Chronic Dis [Internet]. 2016 [cited 2022 Nov 28];13. https://www.cdc.gov/pcd/issues/2016/16_0046.htm .
Cobb-Clark DA, Kassenboehmer SC, Schurer S. Healthy habits: the connection between diet, exercise, and locus of control. J Econ Behav Organ. 2014;98:1–28.
Lassi G, Taylor AE, Mahedy L, Heron J, Eisen T, Munafo MR. Locus of control is associated with tobacco and alcohol consumption in young adults of the Avon Longitudinal Study of parents and children. Royal Soc open Sci. 2019;6(3):181133.
Kesavayuth D, Poyago-Theotoky J, Tran DB, Zikos V. Locus of control, health and healthcare utilization. Econ Model. 2020;86:227–38.
Aikpitanyi J, Okonofua F, Ntoimo LF, Tubeuf S. Demand-side barriers to access and utilization of skilled birth care in low and lower-middle-income countries: a scoping review of evidence. Afr J Reprod Health. 2022;26(9).
Hunter RF, Tang J, Hutchinson G, Chilton S, Holmes D, Kee F. Association between time preference, present-bias and physical activity: implications for designing behavior change interventions. BMC Public Health. 2018;18(1):1388.
Courtemanche C, Heutel G, McAlvanah P. Impatience, incentives and obesity. Econ J. 2015;125(582):1–31.
Weinstein ND. Unrealistic optimism about future life events. J Personal Soc Psychol. 1980;39(5):806.
Weinstein ND. Optimistic biases about personal risks. Science. 1989;246(4935):1232–3.
Article CAS PubMed Google Scholar
Nezlek JB, Zebrowski BD. Implications of the dimensionality of unrealistic optimism for the study of perceived health risks. J Soc Clin Psychol. 2001;20(4):521–37.
Weinstein ND. Unrealistic optimism about susceptibility to health problems. J Behav Med. 1982;5(4):441–60.
Sandroni A, Squintani F. A survey on overconfidence, insurance and self-assessment training programs. Unpublished Rep. 2004;1994–2004.
Sassano M, McKee M, Ricciardi W, Boccia S. Transmission of SARS-CoV-2 and other infections at large sports gatherings: a surprising gap in our knowledge. Front Med. 2020;7:277.
Lehmann EY, Lehmann LS. Responding to patients who refuse to wear masks during the Covid-19 pandemic. J Gen Intern Med. 2021;36(9):2814–5.
Johnson DD, Fowler JH. The evolution of overconfidence. Nature. 2011;477(7364):317–20.
Räikkönen K, Matthews KA, Flory JD, Owens JF, Gump BB. Effects of optimism, pessimism, and trait anxiety on ambulatory blood pressure and mood during everyday life. J Personal Soc Psychol. 1999;76(1):104.
Rozanski A, Bavishi C, Kubzansky LD, Cohen R. Association of Optimism with Cardiovascular events and all-cause mortality: a systematic review and Meta-analysis. JAMA Netw Open. 2019;2(9):e1912200.
Attanasio OP, Kaufmann KM. Education choices and returns to schooling: mothers’ and youths’ subjective expectations and their role by gender. J Dev Econ. 2014;109:203–16.
Lekfuangfu WN, Odermatt R. All I have to do is dream? The role of aspirations in intergenerational mobility and well-being. Eur Econ Rev. 2022;148:104193.
Whitehead R, Currie D, Inchley J, Currie C. Educational expectations and adolescent health behaviour: an evolutionary approach. Int J Public Health. 2015;60(5):599–608.
Caliendo M, Cobb-Clark DA, Uhlendorff A. Locus of control and job search strategies. Rev Econ Stat. 2015;97(1):88–103.
Abay KA, Blalock G, Berhane G. Locus of control and technology adoption in developing country agriculture: evidence from Ethiopia. J Econ Behav Organ. 2017;143:98–115.
Falk A, Becker A, Dohmen T, Huffman D, Sunde U. The preference survey module: a validated instrument for measuring risk, time, and social preferences. Manage Sci. 2022.
Falk A, Becker A, Dohmen T, Enke B, Huffman D, Sunde U. Global evidence on Economic Preferences*. Q J Econ. 2018;133(4):1645–92.
Ruggeri K, Panin A, Vdovic M, Većkalov B, Abdul-Salaam N, Achterberg J, et al. The globalizability of temporal discounting. Nat Hum Behav. 2022;6(10):1386–97.
Boruchowicz C, Lopez Boo F. Better than my neighbor? Testing for overconfidence in COVID-19 preventive behaviors in Latin America. BMC Public Health. 2022;22(1):1009.
Beaman L, Duflo E, Pande R, Topalova P. Female leadership raises aspirations and educational attainment for girls: a policy experiment in India. Science. 2012;335(6068):582–6.
NCES. Parent and Student Expectations of Highest Education Level [Internet]. 2019 [cited 2023 Aug 8]. https://nces.ed.gov/pubs2019/2019015/index.asp .
Download references
Acknowledgements
The authors would like to thank Nicolas Ajzenman, Sebastian Bauhoff, and two anonymous IDB referees for their valuable feedback.
The Inter-American Development Bank (IDB), the Bill and Melinda Gates Foundation, and the Carlos Slim foundation provided funding for this study through the Salud Mesoamerica Initiative. Funders played no role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and affiliations.
Inter-American Development Bank, Social Protection and Health Division, 1300 New York Avenue NW, Washington, DC, USA
Pedro Bernal Lara, Giuliana Daga & Florencia Lopez Boo
Sloan School of Management, Massachusetts Institute of Technology, 100 Main St, Cambridge, MA, USA
Lajos Kossuth
You can also search for this author in PubMed Google Scholar
Contributions
PBL and FLB contributed to the study conception and design. GD and LK prepared the dataset preparation and analyzed it. The first draft of the manuscript was written by GD and LK, with subsequent substantial revisions by PBL and FLB. All authors have read and approved the final manuscript.
Corresponding author
Correspondence to Pedro Bernal Lara .
Ethics declarations
Ethics approval and consent to participate.
The data that supports the findings of this study is property of the Inter-American Development Bank. Data collection was approved by the Health Ministry of El Salvador (MINSAL). All procedures performed to collect the data used in this study followed the usual ethical standards. Informed consent was requested from the household head and each independent survey respondent.
Consent for publication
No identifiable data were included in the analysis, so no consent for publication had to be requested.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Material 1
Supplementary material 2, rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Lara, P.B., Daga, G., Kossuth, L. et al. Do behavioral drivers matter for healthcare decision-making during crises? A study of low-income women in El Salvador during the COVID-19 pandemic. BMC Public Health 24 , 2122 (2024). https://doi.org/10.1186/s12889-024-19039-y
Download citation
Received : 19 October 2023
Accepted : 03 June 2024
Published : 06 August 2024
DOI : https://doi.org/10.1186/s12889-024-19039-y
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Healthcare decision-making
- Behavioral economics
- Low-income setting
- Latin America
- El Salvador
BMC Public Health
ISSN: 1471-2458
- General enquiries: [email protected]

COMMENTS
Examples of literature reviews. Step 1 - Search for relevant literature. Step 2 - Evaluate and select sources. Step 3 - Identify themes, debates, and gaps. Step 4 - Outline your literature review's structure. Step 5 - Write your literature review.
Writing a Literature Review. A literature review is a document or section of a document that collects key sources on a topic and discusses those sources in conversation with each other (also called synthesis ). The lit review is an important genre in many disciplines, not just literature (i.e., the study of works of literature such as novels ...
A literature review is a critical analysis and synthesis of existing research on a particular topic. It provides an overview of the current state of knowledge, identifies gaps, and highlights key findings in the literature. 1 The purpose of a literature review is to situate your own research within the context of existing scholarship ...
Literature reviews take time. Here is some general information to know before you start. VIDEO -- This video is a great overview of the entire process. (2020; North Carolina State University Libraries) --The transcript is included. --This is for everyone; ignore the mention of "graduate students". --9.5 minutes, and every second is important.
Okay - with the why out the way, let's move on to the how. As mentioned above, writing your literature review is a process, which I'll break down into three steps: Finding the most suitable literature. Understanding, distilling and organising the literature. Planning and writing up your literature review chapter.
Your literature review format depends heavily on the kind of manuscript you are writing — an entire chapter in case of doctoral theses, a part of the introductory section in a research article, to a full-fledged review article that examines the previously published research on a topic.
The best proposals are timely and clearly explain why readers should pay attention to the proposed topic. It is not enough for a review to be a summary of the latest growth in the literature: the ...
Demonstrate your knowledge of the research topic. Identify the gaps in the literature and show how your research links to these. Provide the foundation for your conceptual framework (if you have one) Inform your own methodology and research design. To achieve this, your literature review needs a well-thought-out structure.
Writing a literature review requires a range of skills to gather, sort, evaluate and summarise peer-reviewed published data into a relevant and informative unbiased narrative. Digital access to research papers, academic texts, review articles, reference databases and public data sets are all sources of information that are available to enrich ...
This step-by-step guide on how to write an excellent literature review covers all aspects of planning and writing literature reviews for academic papers and theses. How to write a systematic literature review [9 steps] ... This guide covers the definition, purpose, and format of a literature review.
The literature review opening/introduction section; The theoretical framework (or foundation of theory) The empirical research; The research gap; The closing section; We then progress to the sample literature review (from an A-grade Master's-level dissertation) to show how these concepts are applied in the literature review chapter. You can ...
Here, I provide tips on planning and writing a review article, with examples of well-crafted review articles published in The FEBS Journal. The advice given here is mostly relevant for the writing of a traditional literature-based review rather than other forms of review such as a systematic review or meta-analysis, which have their own ...
This page is designed to assist you in writing an annotated bibliography
he simplest thing of all—structure. Everything you write has three components: a beginning, a middle and an e. d and each serves a different purpose. In practice, this means your review will have an introduction, a main body where you review the literature an. a conclusion where you tie things up.
Your report, in addition to detailing the methods, results, etc. of your research, should show how your work relates to others' work. A literature review for a research report is often a revision of the review for a research proposal, which can be a revision of a stand-alone review. Each revision should be a fairly extensive revision.
Steps for Conducting a Lit Review; Finding "The Literature" Organizing/Writing; APA Style This link opens in a new window; Chicago: Notes Bibliography This link opens in a new window; MLA Style This link opens in a new window; Sample Literature Reviews. Sample Lit Reviews from Communication Arts; Have an exemplary literature review? Get Help!
2. MOTIVATE YOUR RESEARCH in addition to providing useful information about your topic, your literature review must tell a story about how your project relates to existing literature. popular literature review narratives include: ¡ plugging a gap / filling a hole within an incomplete literature ¡ building a bridge between two "siloed" literatures, putting literatures "in conversation"
Literature reviews are in great demand in most scientific fields. Their need stems from the ever-increasing output of scientific publications .For example, compared to 1991, in 2008 three, eight, and forty times more papers were indexed in Web of Science on malaria, obesity, and biodiversity, respectively .Given such mountains of papers, scientists cannot be expected to examine in detail every ...
The fundamental rationale of writing a review article is to make a readable synthesis of the best literature sources on an important research inquiry or a topic. This simple definition of a review article contains the following key elements: The question (s) to be dealt with.
A synthesis matrix helps you record the main points of each source and document how sources relate to each other. After summarizing and evaluating your sources, arrange them in a matrix or use a citation manager to help you see how they relate to each other and apply to each of your themes or variables. By arranging your sources by theme or ...
How to create Literature reviews. Growth mindset in high school mathematics: A review of the literature since 2007 Growth mindset has received more focus in schools in the past fifteen years as a possible way to improve various educational outcomes. There are important possible benefits if students believe in the malleability of intelligence and the potential to improve in ability and various ...
Please select a topic for written discussion.Focus specifically on the concerns related to your research study in that area.Identify and gather the appropriate sources.Determine the range of sources required.Create Your OverviewCreate Your Initial DraftRevise and ModifyCreate a literature review in the form of a paper.
Suggests questions to drive primary research based on previous studies. Here are some example topics for writing literature reviews: Exploring racism in "To Kill a Mockingbird," "The Adventures of Huckleberry Finn," and "Uncle Tom's Cabin." Isolationism in "The Catcher in the Rye," "Frankenstein," and "1984".
Articles commonly fall into one of three main categories: Full papers, Communications and Reviews. However, each journal will have further, specific article types, so you should always refer to a journal's specific guidelines while preparing your manuscript.. Full papers are original, unpublished primary research.Extensions of work that has been published previously in short form such as a ...
Section 2 provides a hypothesis development and literature review. Section 3 describes the methodology and measures used in this study. Section 4 presents the analysis and results. Section 5 presents the discussion. Section 6 presents the conclusions of the study. Section 7 outlines the theoretical and practical implications of the study.
Thus, to comprehend how the academic community has been treating such concern a review and synthesis of the literature was undertaken in an identified sample of 986 articles covering the period 1999-2020 (last year included), ultimately down selecting the most relevant 373 peer reviewed articles exploiting a solid methodology in the preparation ...
Background The increase in mpox incidence underscores the crucial need to understand and effectively address prevention, early detection, and agile response to this disease. Therefore, the present study aims to determine the knowledge and attitude towards mpox. Methods A systematic review and comprehensive literature meta-analysis were conducted using prominent databases such as PubMed, Scopus ...
Background/Objectives: This paper reviews three cases of rhegmatogenous retinal detachment (RRD) with giant retinal tear (GRT), focusing on surgical management and outcomes, and synthesizes the current literature on the subject. Methods: We retrospectively analyzed three cases of male patients diagnosed with RRD with GRT at our hospital from April 2022 to November 2023. The patients, aged 57 ...
Abstract Understanding health-seeking behaviors and their drivers is key for governments to manage health policies. A growing body of research explores the role of cognitive biases and heuristics in health and care-seeking behaviors, but little is known about how a context of heightened anxiety and uncertainty might influence these behavioral drivers. This study analyzes the association ...